PCL Injury
Article by John Miller


PCL Injury
Posterior Cruciate Ligament Injury
In the landscape of knee joint issues, a posterior cruciate ligament (PCL) tear emerges as a prevalent concern. This article explores the anatomy, causation, symptoms, and treatment of PCL injuries, enriched with a physiotherapist’s insights and contemporary research.
Anatomy of the PCL
The PCL plays a pivotal role in knee stability, originating from the medial femoral condyle and branching into two bundles—the posteromedial and anterolateral—before attaching to the tibia. Composed of sturdy fibrous material, it restrains joint mobility, averting hyperextension, posterior tibial displacement, and excessive external rotation.
Prevalence of PCL Injuries
While less common than other knee ligament injuries, PCL tears account for 3% to 23% of knee injuries. The PCL’s thickness exceeds that of the ACL, influencing its injury pattern.
Causes of PCL Injuries
PCL injuries typically stem from forced hyperextension or posterior translation of the tibia, prevalent in motor vehicle accidents and sports. They may also co-occur with ACL or MCL injuries.
Symptoms of a PCL Tear
PCL tears can be subtle, with symptoms often more subtle than ACL injuries. Patients may experience more disability than instability, without the notable “pop” associated with knee injuries.
Diagnosing a PCL Tear
Diagnosis involves clinical tests for posterior instability and MRI scans to determine the extent of the ligament damage and associated knee injuries.

Treatment Approaches
Grade I / II Injuries:
Mild to moderate PCL injuries typically respond to non-operative physiotherapy, with favourable outcomes for those who adhere to a rehabilitation programme.
Grade III Injuries:
These might necessitate surgery, depending on functional requirements. Many cases can forego surgery with appropriate rehabilitation.
The Role of Physiotherapy
Physiotherapy for PCL tears aims to:
- Alleviate pain and inflammation
- Normalise joint movement
- Strengthen the knee and lower limb muscles
- Enhance balance and proprioception
- Improve functional capabilities
- Prevent re-injury
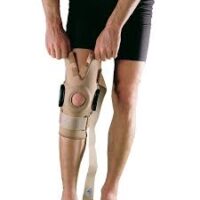
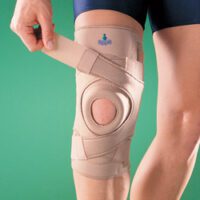
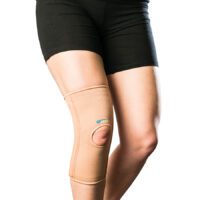
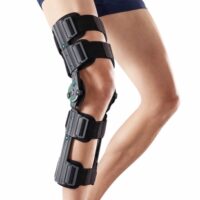
Braces for PCL Tears
Braces offer stability for repairing PCL injuries, with effectiveness varying based on the instability degree. Specially moulded braces are more effective in severe cases.
PCL Surgical Considerations
Deciding on PCL repair surgery involves evaluating factors like knee instability, other ligament damages, and the patient’s level of physical activity.
Post-Surgical Rehabilitation
Optimal outcomes from PCL surgery heavily depend on post-operative physiotherapy, focusing on knee function restoration while safeguarding the repaired ligament.
Sports with High PCL Tear Risks
Sports involving landing, jumping, and twisting have higher PCL injury risks. These include AFL, rugby, basketball, among others.
Preventing PCL Tears
Latest research emphasises neuromuscular and strengthening exercises to prevent PCL injuries. Consultation with a sports physiotherapist for customised prevention strategies is recommended.
Returning to Sport
Athletes with isolated PCL injuries generally return to sport without significant issues. Complications like ACL injuries or posterolateral corner instability or meniscal tears necessitate careful evaluation.
Conclusion
While less common, PCL injuries present significant challenges. Understanding their anatomy, causes, symptoms, and treatments is vital. Effective management through physiotherapy or surgery, under professional guidance, is essential. For a personalised assessment and treatment plan, consulting a sports physiotherapist or knee surgeon is strongly advised.
Seek Professional Advice
If you suspect a PCL injury, consulting a sports physiotherapist or knee surgeon for a comprehensive evaluation and customised treatment plan is crucial. Prompt intervention can greatly improve recovery and facilitate a swift return to daily activities and sports.
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgateArticle by John Miller
Knee Pain Causes
Knee Pain Causes: An In-Depth Guide from a Physiotherapist's Perspective
Knee pain is a common complaint that can significantly impact your daily life. Understanding the causes of knee pain is crucial for effective treatment and prevention. This guide explores various knee pain causes and provides insights from a physiotherapist's perspective.


Common Causes of Knee Pain
Knee pain can stem from a variety of sources, ranging from acute injuries to chronic conditions. Let's explore some common causes:
Ligament Injuries
Ligament injuries are a significant cause of knee pain. These injuries often occur during sports or high-impact activities.
- ACL Injury: The Anterior Cruciate Ligament (ACL) is crucial for knee stability. ACL injuries can result from sudden stops or changes in direction. Symptoms include pain, swelling, and instability. Treatment often involves surgery and rehabilitation.
- PCL Injury: The Posterior Cruciate Ligament (PCL) can be injured in direct trauma to the knee. This injury also leads to pain and swelling, with treatment options ranging from physical therapy to surgery.
- MCL and LCL Sprains: Medial Collateral Ligament (MCL) and Lateral Collateral Ligament (LCL) sprains result from direct blows to the knee. These injuries cause pain and instability, often requiring rest, bracing, and physiotherapy.
Meniscus Injuries
Meniscus tears are another common knee injury. The meniscus is a cartilage that cushions the knee joint.
- Meniscus Tear: This injury often occurs from twisting or rotating the knee while bearing weight. Symptoms include pain, swelling, and difficulty moving the knee. Treatment options vary based on the tear's severity, ranging from rest and physiotherapy to surgery.
- Discoid Meniscus: This congenital condition results in an abnormally shaped meniscus, leading to pain and instability. Treatment may involve surgery to reshape or remove the meniscus.
Kneecap Pain
Several conditions can cause pain in the kneecap area, affecting your ability to perform daily activities.
- Chondromalacia Patella: Also known as "runner's knee," this condition involves the softening and breakdown of the cartilage on the underside of the kneecap. It causes pain and swelling, particularly when walking up stairs or sitting for long periods.
- Patellar Tendinopathy: Also called "jumper's knee," this condition results from overuse, causing pain at the front of the knee. Treatment typically includes rest, physiotherapy, and strengthening exercises.
- Patellofemoral Pain Syndrome: This condition involves pain around the kneecap, often resulting from overuse or misalignment. Treatment includes rest, physiotherapy to improve the patellar tracking, and proper footwear.
Knee Arthritis
Arthritis is a leading cause of knee pain, particularly in older adults. It causes inflammation and stiffness in the joints.
- Knee Osteoarthritis: This degenerative condition involves the wearing down of cartilage, leading to pain and swelling. Treatment includes physiotherapy, medication, and sometimes surgery.
- Rheumatoid Arthritis: This autoimmune condition causes inflammation in the knee joints. It requires medical management and physiotherapy to manage symptoms.
Knee Tendon Injuries
Tendon injuries can result from overuse or sudden, high-impact activities.
- Patellar Tendinopathy: This injury involves the patellar tendon, causing pain below the kneecap. Treatment includes rest, physiotherapy, and strengthening exercises.
- Quadriceps Tendinopathy: This condition affects the tendon connecting the quadriceps muscles to the knee, leading to pain above the kneecap.
Muscle Injuries
Muscle strains and related conditions are common knee pain causes, especially among athletes and active individuals.
- Hamstring Strain: This injury involves the muscles at the back of the thigh. It causes pain, swelling, and difficulty bending the knee. Treatment includes rest, ice, and physiotherapy.
- ITB Syndrome: The Iliotibial Band (ITB) can become tight and inflamed, leading to pain on the outer side of the knee. Stretching and physiotherapy are essential for recovery.
Knee Bursitis
Inflammation of the bursae, small fluid-filled sacs around the knee, can cause significant pain.
- Knee bursitis: Suprapatella bursitis is a common knee bursitis.
- Pes Anserine Bursitis: This condition involves inflammation of the bursa located on the inner side of the knee. It causes pain and swelling, with treatment focusing on reducing inflammation through rest, ice, and physiotherapy.
Children’s Knee Conditions
Young athletes can experience specific knee conditions related to growth and activity levels.
- Osgood Schlatter’s Disease: This condition involves inflammation of the area just below the kneecap where the tendon from the kneecap attaches to the shinbone. It causes pain and swelling, especially during activities.
- Sinding Larsen Johansson Syndrome: This condition affects the growth plate at the bottom of the kneecap, leading to pain and swelling.
Other Knee-Related Conditions
Various other conditions can lead to knee pain, necessitating a broad understanding of potential causes.
- Runner’s Knee: This condition involves pain around the kneecap, often resulting from overuse or misalignment. Treatment includes rest, physiotherapy, and proper footwear.
- Plica Syndrome: Inflammation of the plica, a fold in the knee lining, can cause pain and swelling. Physiotherapy and anti-inflammatory medications are common treatments.
What to Do?
If you're experiencing knee pain, seeking professional advice from a physiotherapist is essential. They can provide a personalised assessment and treatment plan to address your specific needs. Early intervention can significantly improve your outcomes and help you return to a pain-free, active lifestyle.
Conclusion
Understanding the causes of knee pain is the first step towards effective treatment. By addressing the root cause, you can find relief and prevent future issues. Consult a physiotherapist to develop a tailored plan for your knee health.
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgateKnee Pain Causes FAQs
- What are the main causes of knee pain?
- Common causes include ligament injuries, meniscus tears, kneecap pain, arthritis, tendon injuries, muscle strains, and bursitis.
- How can I tell if my knee pain is serious?
- Serious knee pain often involves significant swelling, inability to bear weight, or visible deformity. Consult a physiotherapist or doctor if you experience these symptoms.
- Can knee pain be treated without surgery?
- Yes, many knee pain causes can be treated with physiotherapy, rest, and non-surgical interventions.
- What is the best treatment for knee pain?
- The best treatment depends on the cause. Physiotherapy, rest, strengthening exercises, and sometimes medication or surgery are effective options.
- How can I prevent knee pain?
- Prevent knee pain by maintaining a healthy weight, staying active, wearing proper footwear, and doing strength and flexibility exercises.
- When should I see a physiotherapist for knee pain?
- See a physiotherapist if your knee pain persists for more than a few days, is severe, or affects your ability to perform daily activities.
Related Articles
- Knee Osteoarthritis - Discover effective treatments for knee osteoarthritis.
- ACL Injuries - Learn about symptoms and treatment options for ACL injuries.
- Meniscus Tear - Understand the causes and treatments for meniscus tears.
- Patellar Tendinopathy - Explore treatment options for patellar tendinopathy.
- ITB Syndrome - Find out how to manage and treat ITB syndrome.
- Hamstring Strain - Tips for recovering from a hamstring strain.
- Runner’s Knee - Effective strategies to reduce knee stress for runners.
- Knee Arthroscopy - Learn about this surgical option for knee injuries.
- Quadriceps Tendinopathy - Understand the causes and treatments for this condition.
- Knee Bursitis - Discover ways to reduce inflammation and pain from knee bursitis.
These articles provide detailed information on various knee conditions and their treatments.
Knee Pain FAQs
Knee pain is a widespread issue, impacting individuals of varying ages and lifestyles. Causes range from injuries and wear and tear to conditions like arthritis. This FAQ section aims to provide insights into knee pain, covering diagnosis, ligament issues, ACL injuries, meniscal injuries, age and arthritis concerns, and pain relief methods through exercise and treatment.
Feel free to click on the questions to for deeper discussions into each topic.


Diagnosis Related
How Can I Determine If My Knee Injury Is Serious?
- Learn to assess the severity of your knee injury based on symptoms and situations.
How Can I Identify The Type Of Knee Injury I Have?
- Discover how different knee injuries manifest and what signs to look for.
When Should I Seek a Physiotherapist or Doctor for My Knee Injury?
- Find out the right time to consult professionals for your knee concerns.
Is Knee Clicking a Sign of a Serious Condition?
- Understand what knee clicking indicates about your joint health.
When Should I Consider Getting a MRI for My Knee?
- Learn about the circumstances when an MRI becomes necessary.
Why Has My Knee Suddenly Started Hurting?
- Explore potential reasons behind sudden knee pain.
Why Does My Knee Hurt On The Inner Side?
- Identify causes of inner knee pain and when to seek help.
Knee Ligament Related
What Are The Common Symptoms of a Torn Ligament in the Knee?
- Recognise the signs of a torn knee ligament.
Can I Walk With A Torn Ligament In My Knee?
- Understand the feasibility and risks of walking with a torn ligament.
ACL Related
What are the Consequences of Not Getting Surgery for an ACL Injury?
- Learn about the long-term effects of untreated ACL injuries.
What Are The Symptoms Of An ACL Tear?
- Identify the key signs of an ACL tear.
Meniscus Related
Is Surgery Necessary for a Meniscal Injury?
- Discover when surgery is essential for meniscal injuries.
Can a Torn Meniscus Heal Without Surgery?
- Find out if meniscal tears can heal naturally.
Age & Arthritis Related
At What Age Do Knee Problems Typically Begin?
- Learn about the onset age for common knee problems.
What are the Common Symptoms of Arthritis in the Knee?
- Identify arthritis symptoms in the knee.
Running Related
What are Some Ways that Runners Can Reduce Knee Stress?
- Explore methods for runners to minimise knee stress.
Knee Treatment & Exercise Related
Is Walking Good For Knee Pain?
- Understand the benefits of walking for knee pain.
What are Some Effective Ways to Relieve Knee Pain?
- Discover various methods to alleviate knee pain.
How Much Walking is Recommended for Individuals with Knee Pain?
- Learn the ideal walking duration for those with knee pain.