Spondylosis (Spine Arthritis)
Article by John Miller
Spondylosis (Spine Arthritis)
What is Spondylosis?
Spondylosis, often referred to as spinal arthritis, is a degenerative condition that affects the spine, leading to pain and stiffness, particularly in individuals over fifty. It occurs when the spinal joints experience wear and tear, leading to damage over time. Spondylosis can affect various regions of the spine, including the cervical (neck), thoracic (mid-back), and lumbar (lower back) areas. In severe cases, complications such as sciatica may arise due to pinched nerves.
Why does Spondylosis occur?
Spondylosis primarily results from the natural ageing process. Over time, the spinal joints undergo wear and tear, which can be accelerated by factors such as injuries, poor posture, joint overuse, and excess weight. These factors contribute to permanent changes in the spinal joints, leading to varying degrees of discomfort and pain.
How does Spondylosis affect the body?
The impact of spondylosis varies among individuals. Some may experience no symptoms, while others might suffer from continuous and disabling pain. Common symptoms include intermittent pain or tenderness in the spinal joints, morning stiffness, and visible joint deformities on X-rays. Pain during spinal joint movement is also a typical symptom.
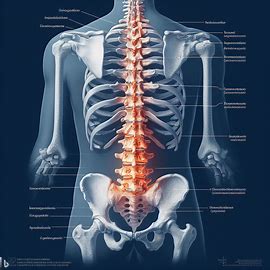
What are the Solutions for Spondylosis?
While there is no cure for spondylosis, modern physiotherapy offers effective management strategies. Physiotherapists conduct a thorough assessment of your condition, considering symptoms, range of motion, strength, posture, and functional limitations. Based on this assessment, a customised treatment plan is developed to improve joint mobility, flexibility, strength, and stability.
Investigations and Diagnosis
Diagnosing spondylosis involves a comprehensive physical examination by a physiotherapist or doctor, often supplemented by imaging techniques like X-rays, MRI, and CT scans. These investigations help confirm the presence of spondylosis and assess the extent of joint damage.
Physiotherapy Management
Physiotherapy management of spondylosis includes several strategies:
- Pain Relief: Manual therapy, joint mobilisation, soft tissue massage, and heat or cold therapy are common techniques used to alleviate pain.
- Exercise Prescription: Specific exercises, including core strengthening and flexibility exercises, are prescribed to improve spinal support and reduce symptoms.
- Education and Self-Management: Patients receive education on lifestyle modifications, posture improvement, and ergonomic principles to help manage their condition effectively.
- Functional Rehabilitation: This aspect focuses on enhancing the ability to perform daily activities, including functional movements, balance training, and gait retraining.
Living with Spondylosis
Managing spondylosis effectively involves respecting your pain and avoiding activities that exacerbate it. Maintaining a healthy weight, engaging in low-impact exercises like walking, swimming, or cycling, and practising core stability exercises are essential. The use of TENS machines for pain relief can also be beneficial.

New Research
Recent studies have shown that exercise-based rehabilitation, when combined with manual therapy, can significantly improve pain management and functionality in individuals with spondylosis. A systematic review highlighted that consistent physiotherapy can lead to better outcomes in reducing pain and improving the quality of life for those affected by spondylosis (Kuo and Tadi., 2023).
What to Do?
For personalised advice and a tailored treatment plan, consulting a professional physiotherapist is crucial. They can guide you through managing your condition, ensuring the best possible outcomes.
Read more: Managing Spinal Conditions | Exercise-Based Rehabilitation for Spinal Health
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgateSpondylosis FAQs
1. What is spondylosis? Spondylosis, or spinal arthritis, is a degenerative condition affecting the spine, leading to pain and stiffness. It commonly occurs in the cervical, thoracic, and lumbar regions due to wear and tear.
2. What causes spondylosis? Spondylosis is primarily caused by age-related wear and tear of the spinal joints. Other factors include injuries, poor posture, joint overuse, and excess weight.
3. How is spondylosis diagnosed? Diagnosis involves a physical examination by a physiotherapist, along with imaging tests like X-rays, MRI, and CT scans to confirm the condition.
4. Can physiotherapy help with spondylosis? Yes, physiotherapy can significantly alleviate pain, improve mobility, and enhance overall functionality through customised treatment plans.
5. What exercises are recommended for spondylosis? Exercises focusing on improving joint mobility, flexibility, strength, and core stability are recommended. Physiotherapists tailor these exercises to individual needs.
6. How can I manage spondylosis at home? Managing spondylosis at home involves lifestyle modifications, posture improvement, activity adaptations, and ergonomic principles. General strength and flexibility, specifically-prescribed physiotherapy and core stability exercises and TENS machines can also be helpful.
Related Articles
- Understanding Spinal Conditions – Learn about various spinal conditions and their management.
- Degenerative Spine Disease – Understand the causes and treatments for degenerative spine disease.
- Managing Back Pain – Practical tips and exercises for managing back pain.
- Sciatica Management – Learn about effective treatments for sciatica caused by spondylosis.
- Core Stability Exercises – Strengthen your core to support your spine and manage spondylosis.
- Posture Improvement – Improve your posture to reduce spinal stress and manage spondylosis.
- Spondylosis: Causes, Symptoms, and Treatment – Explains the causes, symptoms, and treatment options for spondylosis.
- Managing Cervical Spondylosis – Discusses cervical spondylosis management and treatment strategies.
- Lumbar Spondylosis: An Overview – A comprehensive overview of lumbar spondylosis from the National Center for Biotechnology Information.