Foot Pain
Article by John Miller
What are the Different Types of Foot Pain?
Experiencing foot, ankle, or heel pain can significantly impact your daily life, making even simple tasks challenging. Seeking the professional opinion of a physiotherapist can be a vital step towards assessment, accurate diagnosis, and targeted treatment. With a focus on patient goals, a physiotherapist can offer personalised care and advice, ensuring a swift return to your usual activities.
Foot Pain
Foot pain can arise from various sources, and it’s crucial to identify the cause to treat it effectively. Here are five related articles offering in-depth information and advice:
- Plantar Fasciitis Explained: A detailed look at symptoms, causes, and treatments.
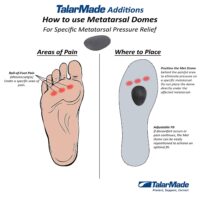
- Metatarsalgia: Forefoot pain and treatment discussed.
- Foot Injury Management: Learn how to manage foot injuries effectively.
- Foot Exercises: Strengthen your feet with these recommended exercises.
- Common Causes of Foot Pain: Tips and strategies to get to the source of your foot pain.
Ankle Pain
Ankle pain, whether acute or chronic, requires proper attention and management. Here are five articles for further exploration:
- Ankle Sprain Recovery: Essential steps to recover from an ankle sprain.
- High Ankle Sprain Information: Understand this specific injury and its treatment options.
- Ankle Injury Prevention: How to prevent ankle injuries in sports and daily life.
Heel Pain
Heel pain can significantly affect your mobility. Explore these articles to understand and address heel pain:
- Dealing with Heel Spurs: Insight into causes and treatments of heel spurs.
- Plantar Fasciitis vs Heel Spurs: A detailed look at differences, symptoms, causes, and treatments.
- Heel Pain in Children (Severs Disease): Addressing heel pain in young athletes.
- Achilles Tendinopathy Care: Effective treatments for Achilles tendon issues.
- Enthesopathy vs Tendinopathy: Discussing the differences of two similar but different sources of heel pain.
How Do You Relieve Foot Pain?
If you’re experiencing foot, ankle, or heel pain, it’s essential to seek professional advice. A physiotherapist can provide you with a comprehensive assessment, diagnose the root cause of your pain, and tailor a treatment plan to meet your specific needs.
For professional care and support, consider booking an appointment with PhysioWorks. Take the first step towards pain-free living today.
By addressing the specific needs of each patient, physiotherapists play a crucial role in pain management and recovery. Whether you’re dealing with an acute injury or chronic pain, expert guidance and treatment can help you return to your favourite activities with confidence.
Common Foot Pain Causes


Various factors, ranging from injuries and tendon problems to degenerative conditions and systemic diseases, can cause foot pain. Some common causes of foot pain include foot injuries, plantar fasciitis, bunions, metatarsalgia, Morton's neuroma, tendon injuries, bone injuries, degenerative conditions like arthritis, biomechanical issues, nerve-related sources such as tarsal tunnel syndrome, and muscle injuries.
Certain systemic conditions like fibromyalgia, lupus, rheumatoid arthritis, and psoriatic arthritis can also contribute to foot pain. This comprehensive list covers a wide range of foot pain causes, encompassing different areas of the foot and various underlying conditions.
Foot Injuries
Tendon Injuries
- Achilles Tendon Rupture
- Achilles Tendinopathy
- FHL Tendinopathy
- Peroneal Tendinopathy
- Tibialis Posterior Tendinopathy
Bone Injuries
- Ankle Fracture (Broken Ankle)
- Stress Fracture
- Stress Fracture Feet
- Severs Disease
- Osteochondritis Dissecans
- Heel Spur
- Shin Splints
Traumatic Ankle Ligament Injuries
Degenerative Conditions
Soft Tissue Inflammation
Biomechanical Conditions
Nerve-Related Sources
Muscle Injuries
Systemic Conditions
Soft Tissue Inflammation
Other Useful Information
Foot, Ankle & Heel Pain FAQs
Introduction
Welcome to PhysioWorks' comprehensive FAQ page on Foot, Ankle, and Heel Pain. Our expert physiotherapists are here to guide you in managing and overcoming discomfort. We’ve organised the FAQs into categories, each with a brief overview and links to in-depth articles, making navigation and understanding easier for you.


Foot Pain
Step into the various causes of foot pain and learn effective ways to relieve discomfort. Understand the impact of activities like barefoot running.
Ankle Injuries
Explore common ankle injuries and how to address them. From sprains to ligament damage, find out the best practices for care and prevention.
Heel Pain
Uncover the reasons behind heel pain and the effective treatments available. This section is particularly useful for understanding conditions like plantar fasciitis and heel spurs.
Achilles Pain
Find out how to manage and treat Achilles tendinopathy, a common concern for athletes and active individuals.
Shin Pain
Learn about shin splints, their causes, and how to alleviate this common issue, especially among runners.
Youth Injuries
Gain insights into youth leg injuries, including growing pains and heel issues in children.
Balance & Proprioception
Enhance your balance and proprioception with our professional advice and exercises.
Related Articles
- Sprained Ankle Treatment & Recovery Guide: Offers detailed advice on how to manage sprained ankles, including immediate recovery steps and physiotherapy treatments.
- Ankle Pain: Effective Management And Treatment Options: Discusses various conditions leading to ankle pain and outlines effective treatment strategies, highlighting the role of physiotherapy in pain reduction and mobility improvement.
- Plantar Fasciitis: Provides an overview of plantar fasciitis, including common causes, treatment options, and related conditions like peroneal tendinopathy and Achilles tendinopathy.
- Achilles Tendinopathy: Focuses on the causes of Achilles tendinopathy, its impact on heel pain, and a range of treatment and prevention strategies.
- Ankle Strapping: Complete Guide To Injury Prevention: Explains the benefits of ankle strapping as a preventative measure against injuries, with a focus on techniques and materials.
- Heel Pain: Explores various causes of heel pain, including tendon injuries, foot injuries, bone injuries, and systemic conditions, alongside recommended treatments.