Lower Back Pain
Article by John Miller
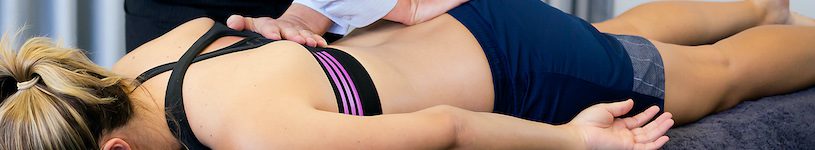
Lower Back Pain
What is Lower Back Pain?
Lower back pain is a widespread issue that can affect anyone at any stage of life. It varies from mild discomfort to a debilitating condition, significantly impacting daily activities and overall quality of life. Understanding the root causes and exploring effective treatment options are key to managing and preventing this common problem.
Why Does Lower Back Pain Occur?
Lower back pain can result from several sources, including:
- Muscle-Related Injuries: Strains, sprains, and fibromyalgia are often due to overuse, poor posture, or sudden movements. These injuries can cause sharp or dull pain that restricts movement.
- Bone & Joint-Related Issues: Conditions such as spondylosis, osteoporosis, and scoliosis can lead to significant pain by affecting the bones and joints in the lower back.
- Disc-Related Injuries: Herniated discs and degenerative disc disease result from wear and tear on the spinal discs, leading to persistent pain.
- Nerve-Related Issues: Sciatica and pinched nerves cause sharp, shooting pain, often radiating down the leg.
- Systemic Diseases: Diseases like ankylosing spondylitis and rheumatoid arthritis can also contribute to lower back pain by causing inflammation in the joints and spine.
Read more: Causes of Back Pain | Muscle Strain and Back Pain

How Do You Investigate Lower Back Pain?
Investigating lower back pain typically involves a thorough assessment by a physiotherapist. This includes reviewing your medical history, conducting physical exams, and possibly using advanced imaging techniques. Real-time ultrasound has become a valuable tool, allowing physiotherapists to observe muscle activation and assess the spine’s condition in real-time.
Read more: Ultrasound in Physiotherapy | Physical Examination for Back Pain
What Are the Solutions for Lower Back Pain?
Effective management of lower back pain often involves a combination of treatments:
- Physiotherapy: A cornerstone in back pain treatment, physiotherapy includes manual therapy, tailored exercises, and education on body mechanics. Strengthening core muscles is particularly vital for supporting the spine and reducing pain.Read more: Physiotherapy for Back Pain | Core Stability Exercises
- Alternative Treatments: Some patients find relief through acupuncture, dry needling, or using a TENS machine, which delivers electrical impulses to alleviate pain.Read more: Acupuncture for Pain Relief | Dry Needling Techniques
- Preventive Measures: Adopting healthy lifestyle habits can prevent lower back pain. These include weight management, proper posture, and safe lifting techniques to avoid strain.Read more: Posture Improvement Tips
FAQs about Lower Back Pain
- Why does lower back pain happen? Lower back pain often occurs due to muscle strain, poor posture, or underlying conditions like herniated discs.Read more: Causes of Back Pain
- How can I relieve lower back pain? Relief can be achieved through physiotherapy, exercise, and in some cases, alternative treatments like acupuncture.Read more: Pain Relief Strategies
- Who is at risk of lower back pain? Anyone can experience lower back pain, but it is more common in people with sedentary lifestyles or those who perform heavy lifting.
- Where does lower back pain usually start? Pain typically starts in the lumbar region and may spread to the buttocks or legs.Read more: Lower Back Pain & Sciatica
- When should I see a physiotherapist for back pain? You should consult a physiotherapist or doctor if the pain persists for more than a few days or if it severely limits your movement.Read more: When to Seek Help for Back Pain
- What exercises help lower back pain? Exercises that strengthen core muscles and improve flexibility are beneficial.Read more: Best Exercises for Back Pain
- How does posture affect lower back pain? Poor posture can strain the lower back muscles, leading to pain.Read more: Posture and Back Pain
- Can stress cause lower back pain? Yes, stress can contribute to muscle tension and pain in the lower back.
- Is lower back pain common during pregnancy? Yes, many women experience lower back pain during pregnancy due to weight gain and changes in posture.Read more: Back Pain in Pregnancy
- What are the latest treatments for lower back pain? New treatments include real-time ultrasound-guided physiotherapy, which improves precision in treatment.Read more: Latest Treatments for Back Pain
Latest Research
Recent studies suggest that integrating lifestyle changes, such as reducing stress and improving diet, with physiotherapy can lead to better outcomes for lower back pain sufferers. New advancements in real-time ultrasound technology have significantly enhanced the accuracy of treatment plans, helping physiotherapists tailor their approach to each patient.
Read more: Low Back Pain Clinical Care Standard
Conclusion
Lower back pain is common, but it’s also manageable. By combining physiotherapy, lifestyle adjustments, and preventive measures, you can significantly reduce or even eliminate your pain. Consult with a physiotherapist to create a personalised treatment plan that addresses your unique needs.
What to Do?
If you’re dealing with lower back pain, don’t wait. Consult with a physiotherapist who can guide you on the best path to recovery. Our team at PhysioWorks is equipped with the latest technology and knowledge to help you get back to living pain-free.
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgateRelated Articles on PhysioWorks
- Core Stability Exercises for Lower Back Pain
- Discover exercises to strengthen your core and support your lower back.
- Physiotherapy for Back Pain
- Learn how physiotherapy can alleviate back pain and prevent future issues.
- Posture and Back Pain: What You Need to Know
- Explore the connection between posture and back pain, with tips to improve your posture.
- Acupuncture for Back Pain Relief
- Understand how acupuncture may help reduce back pain.
- Real-Time Ultrasound in Physiotherapy
- Discover the benefits of using real-time ultrasound in diagnosing and treating lower back pain.
- Back Pain During Pregnancy
- Explore common causes and solutions for back pain during pregnancy.
- Lower Back Pain
- Learn about common causes, symptoms, and treatment options for lower back pain.
- Lower Back Pain Causes and Treatments
- Explore various causes of lower back pain and available treatment options.
- Lower Back Pain Remedies
- Discover home remedies and medical treatments for lower back pain.