Patella Dislocation
Article by John Miller

Patella Dislocation and Subluxation: What’s the Difference?
Patella dislocation occurs when the kneecap (patella) completely moves out of its normal position in the femur’s groove. This can result from trauma, such as a twisting injury or a direct blow to the knee. It frequently affects athletic teenagers and young adults but can occur in anyone.
What is Patella Dislocation?
Patella dislocation happens when the kneecap moves out of its groove at the end of the femur. Often, the kneecap is displaced outwardly, causing significant damage to the muscles and ligaments inside the knee. This condition is more common in athletic individuals but can occur due to various reasons.
Understanding Patella Subluxation
Unlike a complete dislocation, patella subluxation is a partial displacement of the kneecap. Although less severe, it still causes discomfort and instability, affecting the knee’s function.
Contributing Factors
Several factors can make an individual more prone to patella dislocation, including:
- Previous knee injuries
- Anatomical irregularities, such as a shallow femoral groove
- Muscle imbalances, especially weak inner quadriceps
- Tight leg muscles, like the iliotibial band
Recognising Symptoms
Symptoms of patella dislocation include:
- Visible misalignment of the kneecap, usually to the outside
- Sharp pain and swelling
- A sensation of instability or weakness in the affected leg
The Diagnostic Process
A physiotherapist or doctor will perform a physical examination, supplemented by imaging tests like X-rays or MRIs, to assess the damage to surrounding structures and tailor the treatment plan.
Treatment Strategies
Immediate Management
If the kneecap doesn’t realign naturally, medical intervention is necessary to reposition it.
Emphasis on Physiotherapy
Physiotherapy is crucial in rehabilitation, focusing on:
- Reducing pain and inflammation
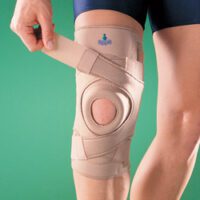
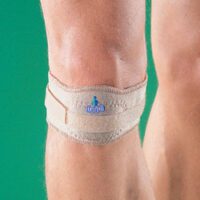
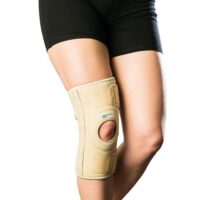
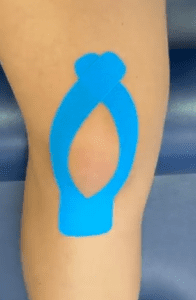
- Stabilising the patella through taping or bracing
- Restoring joint mobility
- Strengthening the knee and lower limb muscles
- Enhancing balance and proprioception
Recovery typically spans 8 to 12 weeks. However, everyone has different needs, so it’s important to discuss your specific requirements with your physiotherapist.
Surgical Considerations
Surgery is reserved for severe cases with significant bone or ligament damage. Post-surgical physiotherapy is essential for a full recovery.
Preventing Recurrent Dislocations
Active Rehabilitation
A structured rehabilitation program is vital to reduce the risk of re-dislocation. Physiotherapists customise these programs to address individual needs, focusing on muscle strengthening and joint stability.
Utilising Braces and Stretching Tools
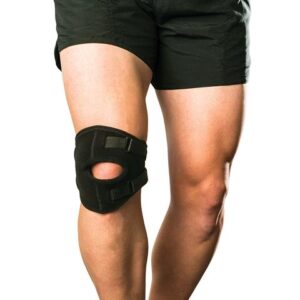
A patellofemoral brace can offer additional support during activities. Regular use of an ITB roller aids in maintaining muscle flexibility.
Returning to Sports
For athletes, the journey back to sports requires specialised exercises to regain strength and stability. Physiotherapists play a key role in designing these sport-specific programs.
Conclusion: Prioritising Knee Health
Patella dislocation, though potentially debilitating, requires prompt and effective management. Early intervention, comprehensive physiotherapy, and preventive strategies are critical for a successful recovery and return to an active lifestyle. Consulting a professional physiotherapist ensures a tailored recovery plan and reduces the risk of future knee problems.
What to Do?
To safeguard your knee health, actively participate in your treatment and follow preventive measures. Your physiotherapist is your guide, helping you achieve optimal recovery and maintain an active, fulfilling life.
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgatePatella Dislocation FAQs
Q1: What is patella dislocation? A: Patella dislocation occurs when the kneecap moves out of its normal position in the femur’s groove, often due to trauma.
Q2: What are the symptoms of patella dislocation? A: Symptoms include visible kneecap misalignment, sharp pain, swelling, and a feeling of instability in the affected leg.
Q3: How is patella dislocation diagnosed? A: Diagnosis involves a physical examination and imaging tests like X-rays or MRIs to assess damage to the knee structures.
Q4: What are the treatment options for patella dislocation? A: Treatment includes immediate repositioning of the kneecap, physiotherapy to reduce pain and inflammation, and possibly surgery for severe cases. Strengthening, protection, kinesio taping and patella braces are potentially useful.
Q5: How can recurrent patella dislocations be prevented? A: Preventive measures include a structured rehabilitation program, use of a patellofemoral brace, and regular muscle flexibility exercises. Ask your physio for specific advice
Q6: Can athletes return to sports after a patella dislocation? A: Yes, with specialised exercises designed by physiotherapists to regain knee strength and stability, athletes can return to sports.
Related Articles
- Knee Pain and Injuries – Learn about various knee injuries and how to manage them effectively.
- Anterior Cruciate Ligament (ACL) Injuries – Discover the causes, symptoms, and treatments for ACL injuries.
- Meniscus Tears – Understand the types of meniscus tears and the best treatment approaches.
- ITB Syndrome – Explore the causes and management strategies for Iliotibial Band Syndrome.
- Patellofemoral Pain Syndrome – Find out more about this common knee condition and its treatment options.
- Post-Surgery Physiotherapy – Get insights into the importance of physiotherapy following knee surgery.
- Knee Bracing for Support – Understand how knee braces can aid in recovery and prevent injuries.
- Sports Injury Prevention – Discover tips and techniques to prevent sports-related injuries.
- Balance and Proprioception Training – Learn exercises to improve balance and proprioception for better knee stability.
Each article offers valuable insights into managing knee health and preventing injuries, making them essential reads for anyone dealing with knee issues.
Social Media
Stay connected with us on social media for valuable tips on managing patellar pain and improving knee health. Access advice from experienced physiotherapists to keep your body moving smoothly.