Pinched Nerve
Article by John Miller

What is a Pinched Nerve?
A pinched nerve occurs when surrounding structures injure and compress a nerve. For instance, the sciatic nerve often gets pinched. This compression damages the nerve and triggers pain and other symptoms.
Commonly Pinched Nerves
Lower Back Pinched Nerve
In your lower back, a disc bulge, arthritis spur, or ligament swelling can pinch the sciatic nerve. This causes leg pain, often referred to as sciatica.
Nerve Compression in the Spinal Canal
Inside your spinal column, neural compression can occur from space occupying causes: eg disc bulge, spinal stenosis, inflammation or even tumours. This leads to various symptoms like nerve pain, sensory loss, and muscle weakness, disrupting normal nerve function.
Neck Pinched Nerve
Nerves in your neck also frequently get pinched. The medical term for a pinched nerve in the neck is cervical radiculopathy. This results in symptoms like arm pain and weakened reflexes. These symptoms can mimic other arm issues like carpal tunnel syndrome and tennis elbow. In such cases, consult a qualified healthcare provider for a comprehensive evaluation.
Peripheral Pinched Nerves
Nerves can get pinched anywhere in your body, often in restricted spaces like tunnels. Carpal tunnel syndrome is a classic example, involving a pinched nerve in your wrist’s front.
Diagnosing a Pinched Nerve
A pinched nerve sends pain signals via spinal cord nerves to the brain. To identify the pinched nerve’s location, your doctor or physiotherapist will evaluate your symptoms. They might also suggest further tests like X-rays, CT scans, MRIs, or nerve conduction studies.
Pinched Nerve Symptoms
Symptoms of a pinched nerve can vary widely. These include nerve pain, unusual sensations like pins and needles, muscle weakness, and reduced reflexes. In extreme cases, you might lose bladder or bowel control. If you notice these symptoms, seek medical help urgently. The longer the nerve stays pinched, the worse the outcomes could be.
If you experience these symptoms, please consult your doctor or physiotherapist without delay.
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgateArticle by John Miller
What is Pain?
Pain is a critical signal from the body indicating injury or distress. Whether you experience acute or chronic pain, understanding its nature is the first step towards effective treatment. This FAQ page, from a physiotherapist’s perspective, will explain the types, causes, and treatments for various pain conditions.

Why does pain occur?
Pain occurs when nociceptors, specialised nerve cells, detect harmful stimuli such as heat, pressure, or chemical changes. These receptors trigger a series of signals through nerve fibres to the brain, where they are interpreted as pain. This response serves as an alert system, helping us avoid further injury.
How is pain transmitted in the body?
The transmission of pain signals begins with receptor nerve cells at the site of injury. These signals travel via nerve fibres (A-beta, A-delta, and C fibres) through the spinal cord to the brain. The speed and type of nerve fibres involved influence the nature of pain—whether sharp, acute, or chronic.
What is the difference between acute and chronic pain?
Acute pain typically occurs suddenly due to injury or illness and resolves as the body heals. Chronic pain, however, lasts longer than three months, often persisting even after the original injury or illness has healed. Chronic pain can involve complex interactions between the nervous system and psychological factors.
More info: Chronic Pain Explained
How can physiotherapy help in managing pain?
Physiotherapy uses a combination of manual therapy, tailored exercises, and education to manage pain. Techniques like joint mobilisation, massage, and specific exercise programs improve muscle strength and flexibility, reducing pain and preventing further injuries.
Physiotherapy generally focuses on non-invasive, drug-free methods for managing pain and improving function. However, in some cases, pharmacological intervention, such as pain relievers or anti-inflammatory medications, may be recommended alongside physiotherapy. This is typically decided by a doctor or pharmacist and is used to manage acute or chronic pain, allowing patients to engage more effectively in physiotherapy exercises. Common medications may include NSAIDs (non-steroidal anti-inflammatory drugs), muscle relaxants, or nerve pain medications.
Learn more about physiotherapy treatments for pain
What is nerve pain, and how is it treated?
Nerve pain (neuropathic pain) is caused by damage or irritation to the nerves and can feel like shooting, burning, or stabbing sensations. Physiotherapy can help manage nerve pain through exercises, manual therapy, and education on nerve mobilisation techniques.
Discover more about nerve pain management
What role does the brain play in pain perception?
The brain plays a significant role in interpreting pain signals. It processes sensory input from nerve cells and can even modulate the intensity of pain based on psychological and emotional factors, which is why pain can feel worse under stress or anxiety.
Can stress or anxiety worsen physical pain?
Yes, stress and anxiety can significantly impact the perception of pain. When stressed, the body releases hormones like cortisol, which can heighten the sensitivity to pain. Additionally, anxiety can lead to muscle tension, which may aggravate existing pain conditions. Managing stress through relaxation techniques, exercise, and cognitive behavioural therapy (CBT) can help reduce the impact of stress on pain.
What can I do at home to manage pain?
Home-based strategies to manage pain include applying ice or heat, engaging in gentle exercise, and practising relaxation techniques such as deep breathing or meditation. Physiotherapists can provide personalised home exercise programs to improve mobility and reduce pain.
Conclusion
Pain, whether acute or chronic, impacts every aspect of life. With tailored physiotherapy techniques such as manual therapy, exercise, and education, pain can be managed effectively. Seek a doctor or physiotherapist's guidance for a personalised pain management plan.
Rochedale - Call 38410277
Book Online: RochedaleSalisbury - Call 32751044
Book Online: SalisburySandgate - Call 32691122
Book Online: SandgateRelated Articles
- Chronic Pain – Discover effective physiotherapy treatments for chronic pain.
- Nerve Pain – Learn about the causes of nerve pain and how to manage it.
- Post-Exercise Muscle Soreness – Understand why your muscles hurt after exercise and how to prevent it.
- Pain Management – Explore physiotherapy techniques for managing various types of pain.
- Spinal Pain – Learn about spinal pain causes and treatment options.
- Back Pain Relief – Discover effective ways to alleviate back pain.
- Joint Pain – Find out how physiotherapy can help with joint pain.
- Manual Therapy – Learn about hands-on techniques to relieve pain.
- Exercise for Pain Relief – Find out how specific exercises can manage chronic pain.
- Massage Therapy – Learn how massage therapy can alleviate muscle and joint pain.
- Understanding Chronic Pain: Causes and Treatments – Discusses the complexities of chronic pain and its management options.
- Nerve Pain Relief: Best Practices – Offers insights into managing nerve pain with both medication and physiotherapy techniques.
- Physiotherapy and Pain Management – Explains the role of physiotherapy in addressing both acute and chronic pain.
Follow Us for Free Tips
Stay updated with the latest tips on managing pain by following us on social media. Our team regularly shares valuable insights to help you stay pain-free and healthy. Follow us on Facebook, Instagram, and Twitter to get expert advice and physiotherapy tips tailored to your needs.
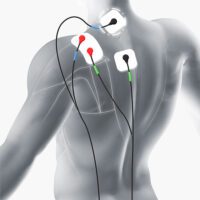
TENS Machine FAQs


TENS & EMS Machine FAQs
Navigating the world of TENS and EMS machines can be overwhelming with all the available options and information. Our comprehensive TENS Machine FAQs are here to guide you through everything you need to know. Whether you’re considering purchasing a TENS or EMS machine, seeking the best practices for electrode placements, or simply curious about the differences between these devices, this resource has got you covered. Learn how these revolutionary devices might help manage pain and enhance your well-being.
What is a TENS Machine?
A TENS machine (Transcutaneous Electrical Nerve Stimulation) is a device that uses low-voltage electrical current to relieve pain. It's a popular option for managing chronic pain and post-operative discomfort.
- TENS Machine Info: Learn about how TENS machines work, their benefits, and potential side effects.
How to Use a TENS Machine
Using a TENS machine correctly is crucial for effective pain relief. Follow these guidelines for optimal results.
- How to Use a TENS Machine: Step-by-step instructions for safe and effective TENS machine use.
What are the Most Effective TENS Machine Electrode Placements?
Proper electrode placement is key to getting the most out of your TENS machine. This eBook provides detailed instructions.
- Effective Electrode Placements (eBook): Explore various electrode placements for different types of pain relief.
What is EMS (Electric Muscle Stimulation)?
EMS machines stimulate muscle contractions using electrical impulses. They are often used for rehabilitation and strength training.
- EMS Machine Info: Discover how EMS machines work and their benefits for muscle recovery and strengthening.
Buy a TENS or EMS Machine
Considering purchasing a TENS or EMS machine? Here's what you need to know about buying these devices.
- Buy TENS Machines: Explore different TENS machine models and their features.
- Buy EMS Machines: Find the right EMS machine for your needs.
- Buy TENS Electrodes & Leads: Ensure you have the necessary accessories for your TENS machine.
TENS Machine – Private Health Insurance Rebate
Find out if your health insurance covers the cost of a TENS machine.
- Health Insurance Rebate Info: Learn about private health insurance rebates for TENS machines.
Pain FAQs
Understanding Pain: Exploring its Types, Causes, and Impact on Well-being Pain can be complex. Understanding its different types and causes can help you manage it better.
- Understanding Pain: Comprehensive information on different types of pain and their causes.
What is Pain? Pain is a signal in your nervous system that something might be wrong. It is an unpleasant sensation and emotional experience linked to tissue damage.
- What is Pain?: Detailed explanation of pain and its mechanisms.
What is Nerve Pain? Nerve pain, or neuropathic pain, occurs when there is damage or dysfunction in the nerves themselves.
- What is Nerve Pain?: Insights into the causes and treatments of nerve pain.
What is Chronic Pain? Chronic pain persists for months or even years. It can significantly impact your quality of life.
- Chronic Pain Info: Information on managing chronic pain effectively.
What Causes Post-Exercise Muscular Pain? Learn about the reasons behind muscle soreness after exercise and how to alleviate it.
- Post-Exercise Pain: Tips on managing muscle pain after workouts.
Conclusion
TENS and EMS machines may offer significant potential for pain management and muscle recovery. Always consult with a healthcare professional to ensure these devices are suitable for your needs. Explore the related articles for more in-depth information on managing pain and enhancing your health and well-being.
IMPORTANT
A TENS machine and an EMS machine are electronic medical devices. Always read the label and instruction manual. A TENS machine may assist you in modest short-term pain relief. Consult your doctor or healthcare professional before use and if symptoms persist. Use only as directed.
TENS Machine FAQs
- What is a TENS Machine? A TENS machine uses low-voltage electrical currents to relieve pain by stimulating nerves.
- How does a TENS Machine work? It sends electrical impulses through electrodes placed on the skin to disrupt pain signals sent to the brain.
- What conditions can a TENS Machine help with? TENS machines can help with chronic pain, arthritis, post-operative pain, and more.
- Are there any side effects of using a TENS Machine? Generally, TENS machines are safe, but some people might experience skin irritation or discomfort at electrode sites.
- How do I place the electrodes for a TENS Machine? Electrode placement depends on the area of pain. Refer to the device manual or consult a healthcare provider.
- Can I use a TENS Machine while pregnant? It is advised to consult a healthcare provider before using a TENS machine during pregnancy.
Related Articles
- Understanding Pain Discusses different types of pain and their causes, providing a deeper insight into pain management.
- TENS Machine Info Detailed information on how TENS machines work and their benefits.
- How to Use a TENS Machine A step-by-step guide on using TENS machines effectively.
- Effective Electrode Placements (eBook) Explains optimal electrode placements for various types of pain relief.
- EMS Machine Info Provides insights into how EMS machines work and their benefits for muscle recovery.
- Buy TENS Machines Explore different models and features of TENS machines available for purchase.
- Chronic Pain Info Information on chronic pain management strategies.
- What is Nerve Pain? Insights into the causes and treatments of nerve pain.
- Post-Exercise Pain Tips on managing muscle soreness after exercise.
- Health Insurance Rebate Info Information on private health insurance rebates for TENS machines.
These related articles will provide you with a broader understanding of pain management and the use of TENS and EMS machines.