Temporomandibular Disorder (TMD)
Article by John Miller
Temporomandibular Disorder (TMD)
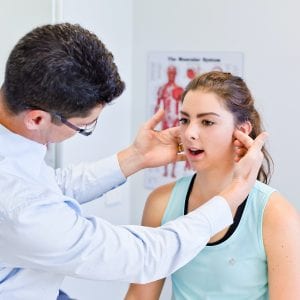
Temporomandibular Disorder (TMD) affects the temporomandibular joint (TMJ), which is essential for daily activities like eating, talking, and expressing emotions. Problems with this joint can significantly impact your quality of life.
Recognising TMD Symptoms
TMJ dysfunction symptoms can manifest in various ways. Common signs include:
- Jaw pain, clicking or popping
- Grinding sounds
- Limited or deviating jaw opening
- Challenges in fully clenching the jaw
Beyond jaw pain, TMD may cause headaches, ear discomfort, dizziness, neck pain, difficulty eating, and tinnitus (Vierola et al., 2012).
How Do You Fix TMD Issues?
A thorough assessment is crucial for diagnosing TMJ dysfunction. TMJ physiotherapists, dental professionals, or oral maxillofacial surgeons use various techniques, including imaging like X-rays, CT scans, or MRIs. They evaluate jaw motion, muscle tension, your bite, and TMJ coordination.
Avoiding Aggravating Activities
Until you see a TMJ physiotherapist or dentist, avoid actions that may worsen symptoms, such as wide yawning, biting hard foods, chewing gum, stressful situations, and clenching objects in your mouth.
Common Treatments for TMD
Physiotherapy plays a pivotal role in treating TMJ disorders. Treatments may include:
- Education on the condition and strategies to alleviate strain
- Soft tissue massage and trigger point release
- Manual therapy to improve mobility and reduce tension
- Exercise therapy for strengthening and stretching
- Heat/cold therapy, ultrasound, and stimulation for pain relief
- Posture, jaw positioning, and ergonomic adjustments
- Dry needling and acupuncture
- Behavioural strategies to manage stress and reduce harmful habits
Each treatment plan is tailored to the individual’s needs, often involving collaboration with dental and healthcare professionals.
Addressing Locked Jaw
For a locked jaw, treatment varies. Physiotherapists may perform gentle manipulation, or in more severe cases, an oral surgeon might be consulted for advanced procedures.
Does TMD Go Away?
TMJ dysfunction requires a personalised approach. Consulting a TMJ physiotherapist is essential for an effective treatment plan. They will guide you through exercises and therapies based on your specific needs. Don’t hesitate to seek professional advice for better management of your TMJ disorder.
What to Do?
If you suspect you have TMD, seek the professional advice of your physiotherapist. They can provide a comprehensive assessment and tailor a treatment plan to your needs, ensuring the best possible outcome for your jaw health.
Conclusion
TMJ dysfunction can significantly impact your daily life, but with the right treatment and management strategies, you can alleviate symptoms and improve your quality of life. Consulting a TMJ physiotherapist is the first step towards better jaw health.
FAQs about TMD
1. What is TMJ dysfunction syndrome? TMJ dysfunction syndrome refers to problems with the temporomandibular joint, which can cause jaw pain, clicking, and other symptoms.
2. What are common symptoms of TMD? Common symptoms include jaw pain, clicking sounds, grinding, limited jaw movement, headaches, ear discomfort, dizziness, neck pain, and tinnitus.
3. How is TMJ dysfunction diagnosed? Diagnosis involves a thorough assessment by a physiotherapist, dentist, or oral maxillofacial surgeon, often using imaging techniques like X-rays, CT scans, or MRIs.
4. What treatments are available for TMJ dysfunction? Treatments include physiotherapy, soft tissue massage, manual therapy, exercise therapy, heat/cold therapy, dry needling, acupuncture, and behavioural strategies.
5. Can TMJ dysfunction be cured? While TMJ dysfunction may not be completely curable, it can be effectively managed with a personalised treatment plan developed by a physiotherapist.
6. When should I see a physiotherapist for TMJ issues? You should see a TMD physiotherapist or dentist if you experience persistent jaw pain, clicking sounds, limited jaw movement, or other symptoms of TMD.
Related Articles
- TMJ FAQs – Discover answers to common questions about TMJ disorders, including symptoms and treatments.
- Jaw Pain – Learn about the various treatment options for TMJ disorders and how physiotherapy can help.
- TMD Treatment – Explore different methods to manage TMJ dysfunction effectively.
- What Causes TMJ? – Discusses the root causes of TMJ dysfunction and factors that contribute to this condition.
- Headache, Neck & Jaw – Understand the connection between TMJ issues and other physical discomforts like headaches and neck pain.
- TMJ Headache – Focuses on headaches resulting from TMJ disorders and offers insights into treatment options.
- Dry Needling for TMJ – Provides information on how dry needling can be an effective treatment for TMJ pain.
- Mayo Clinic – TMJ Disorders – Offers a comprehensive overview of TMJ disorders, including symptoms and treatment options.



