Sprained Ankle
Article by John Miller

Sprained Ankle
Recovery from a Physiotherapist’s Perspective
A sprained ankle, a common but often misunderstood injury, affects both athletes and the general population. As a physiotherapist, my goal is to guide you through understanding the mechanics, symptoms, and effective treatment of this injury.
The Mechanics Behind the Injury
An ankle sprain occurs when the ligaments, the strong fibrous tissues connecting bones, are overstretched. Typically resulting from accidents, uneven terrain, or unsuitable footwear, sprains can range from mild to severe, with potential bone fractures.
Identifying the Symptoms
Symptoms vary from mild pain and swelling to severe discomfort, bruising, and even a popping sound at the injury moment. Difficulty in weight-bearing or walking normally often necessitates temporary support, such as crutches or a supportive boot.
The Importance of an Accurate Diagnosis
Proper diagnosis involves a detailed examination, assessing tenderness, swelling, and motion range. Sometimes, X-rays or MRI scans are necessary to rule out fractures and assess soft tissue damage.
Which Ligaments Are Involved?
Most ankle sprains involve the lateral ligaments on the ankle’s outside, including the anterior talofibular, calcaneofibular, and posterior talofibular ligaments. The medial deltoid ligament and, in high ankle sprains, the tibia and fibula ligaments can also be involved, leading to more complex injuries.
The Consequences of Misdiagnosis
Misdiagnosis can lead to chronic ankle instability and potentially require intensive treatment or surgery. Thus, accurate identification and treatment planning are crucial.
Physiotherapy Treatment for a Sprained Ankle
Immediate Measures for Recovery
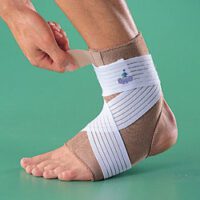
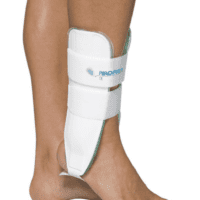
- Managing Pain and Inflammation: Rest, ice, compression, and elevation (RICE) are vital first steps. Ankle strapping, moon boots, or braces may be prescribed.
Restoring Mobility
- Gentle Exercises: As inflammation reduces, tailored exercises under physiotherapist supervision aim to restore full motion range.
Strengthening the Area
- Targeted Exercises: These focus on muscles around the ankle and calf to improve stability and prevent future injuries, adjusted in intensity to match recovery stages.
Enhancing Proprioception and Balance
- Proprioceptive Training: Critical for regaining ankle stability, these exercises improve the body’s awareness of its position in space.
Preparing for Athletic Demands
- Sport-Specific Training: For athletes, treatment includes exercises tailored to the dynamic demands of their sport.
The Road Back to Full Activity
- Gradual Training Resumption: Monitoring and gradually increasing exercise intensity ensures a successful transition back to activities.
Final Stages: Return to Competition
- Full Recovery Preparation: The focus is on regaining pre-injury strength, function, and flexibility.
Recovery Timelines for Sprained Ankles
Recovery is highly individual, with ligaments typically healing within six weeks. However, full recovery depends on restoring strength, motion, and function. Mild grade I injuries will rehabilitate quicker than Grade III ruptures that may require longer immobilisation or ligament reconstruction surgery.
The Risks of Neglect
Untreated sprains can lead to chronic ankle issues. Adhering to a structured physiotherapy plan is essential to avoid long-term problems.
Conclusion
A sprained ankle demands prompt and effective physiotherapy treatment. Early consultation with a physiotherapist ensures a customised treatment plan, leading to quicker recovery and minimising future ankle issues. Remember, each ankle sprain is unique; professional guidance is key to a successful recovery.
New Research Insights
Recent studies emphasise the importance of tailored rehabilitation programs. According to a 2022 study, exercise based physiotherapy significantly enhances recovery outcomes, reducing the risk of re-injury and chronic instability. The integration of balance and proprioceptive training has been highlighted as particularly effective in promoting long-term ankle health.
What to do?
If you’re experiencing symptoms of a sprained ankle, don’t hesitate to seek professional advice. As a physiotherapist, I can provide you with a tailored treatment plan, ensuring the best possible outcome for your recovery. Remember, timely and appropriate treatment is the key to getting back on your feet confidently and safely.
Related Articles
- Ankle Injury Treatment: Discover the various treatment methodologies for ankle injuries, including physiotherapy techniques. It expands on the treatment section of the original article.
- Preventing Ankle Injuries: Tips on how to prevent ankle injuries in sports and daily activities. Prevention is crucial for those who’ve previously experienced a sprained ankle or are at high risk.
- Sports Injuries and Physiotherapy: Explore how physiotherapy can address various sports injuries, including ankle sprains. This is particularly relevant for the athletic readership.
- Balance Exercises: Find out about exercises that improve balance, which is essential for ankle stability post-injury. This supports the section on proprioceptive training and balance enhancement.
Common Causes of Ankle Pain
Introduction
Welcome to our detailed guide on the common causes of ankle pain. As physiotherapists, we understand how various conditions and injuries can lead to discomfort in your ankle. From sprains to degenerative diseases, this guide aims to provide clear insights for the general public on navigating these issues.


Sprained Ankles and Syndesmosis Injuries
Sprained ankles, including syndesmosis injuries, are among the most common issues we encounter. These injuries can range from mild ligament stretches to severe tears, impacting your mobility and quality of life. Understanding the specifics of each type is crucial for effective treatment and timely recovery.
Ankle Tendinopathies
Tendinopathies, such as those affecting the Achilles and tibialis posterior tendons, are common in active individuals. These conditions arise due to overuse or trauma, leading to pain and swelling in the affected area. Targeted physiotherapy can significantly aid in recovery and prevent future injuries.
Posterior Ankle Conditions
Conditions like posterior ankle impingement and retrocalcaneal bursitis can cause significant pain, especially during physical activities. Recognising these conditions early and starting appropriate treatment is vital for maintaining ankle health and functionality.
Ankle Arthritis
Arthritis in the ankle, often a result of wear and tear or injury, leads to joint pain and stiffness. Early intervention and proper management, including physiotherapy, are essential to slow its progression and manage symptoms effectively.
Biomechanical Conditions
Abnormal foot and ankle biomechanics can lead to various issues, from pain during weight-bearing to nerve compression. Understanding and treating these conditions are crucial for restoring normal function and preventing further complications.
Systemic Conditions That May Cause Ankle Pain
Systemic diseases such as rheumatoid arthritis can manifest as ankle pain. It's important to address these underlying conditions to effectively manage ankle symptoms.
Conclusion
Ankle pain can arise from a multitude of causes, each requiring a unique approach to treatment. If you're experiencing ankle discomfort, we recommend consulting a physiotherapist or doctor for a thorough evaluation. A personalised care plan can significantly improve your quality of life and mobility.
Related Articles
- Sprained Ankle Treatment & Recovery Guide - This article provides comprehensive information on managing pain and inflammation for a sprained ankle, including initial RICE steps and exercises for restoring mobility.
- Anterior Ankle Impingement: Causes, Treatments, Tips & Guide - Offers insights into the causes of anterior ankle impingement, its treatments, and practical tips for management.
- Posterior Ankle Impingement: Causes & Treatments - Explains the condition of posterior ankle impingement, its causes, and available treatment options.
- Tibialis Posterior Tendinopathy - Discusses the condition affecting the tibialis posterior tendon, symptoms, and implications for foot arch pain and ankle stability.
- Achilles Tendinopathy - Answers frequently asked questions about foot and ankle pain associated with Achilles tendinopathy and provides an overview of tendon injuries.
- How To Strap An Ankle - Guides on the correct techniques and types of tape for ankle strapping to prevent or manage ankle injuries.
Foot, Ankle & Heel Pain FAQs
Introduction
Welcome to PhysioWorks' comprehensive FAQ page on Foot, Ankle, and Heel Pain. Our expert physiotherapists are here to guide you in managing and overcoming discomfort. We’ve organised the FAQs into categories, each with a brief overview and links to in-depth articles, making navigation and understanding easier for you.


Foot Pain
Step into the various causes of foot pain and learn effective ways to relieve discomfort. Understand the impact of activities like barefoot running.
Ankle Injuries
Explore common ankle injuries and how to address them. From sprains to ligament damage, find out the best practices for care and prevention.
Heel Pain
Uncover the reasons behind heel pain and the effective treatments available. This section is particularly useful for understanding conditions like plantar fasciitis and heel spurs.
Achilles Pain
Find out how to manage and treat Achilles tendinopathy, a common concern for athletes and active individuals.
Shin Pain
Learn about shin splints, their causes, and how to alleviate this common issue, especially among runners.
Youth Injuries
Gain insights into youth leg injuries, including growing pains and heel issues in children.
Balance & Proprioception
Enhance your balance and proprioception with our professional advice and exercises.
Related Articles
- Sprained Ankle Treatment & Recovery Guide: Offers detailed advice on how to manage sprained ankles, including immediate recovery steps and physiotherapy treatments.
- Ankle Pain: Effective Management And Treatment Options: Discusses various conditions leading to ankle pain and outlines effective treatment strategies, highlighting the role of physiotherapy in pain reduction and mobility improvement.
- Plantar Fasciitis: Provides an overview of plantar fasciitis, including common causes, treatment options, and related conditions like peroneal tendinopathy and Achilles tendinopathy.
- Achilles Tendinopathy: Focuses on the causes of Achilles tendinopathy, its impact on heel pain, and a range of treatment and prevention strategies.
- Ankle Strapping: Complete Guide To Injury Prevention: Explains the benefits of ankle strapping as a preventative measure against injuries, with a focus on techniques and materials.
- Heel Pain: Explores various causes of heel pain, including tendon injuries, foot injuries, bone injuries, and systemic conditions, alongside recommended treatments.