Pes Planus (Flat Feet)
Article by John Miller
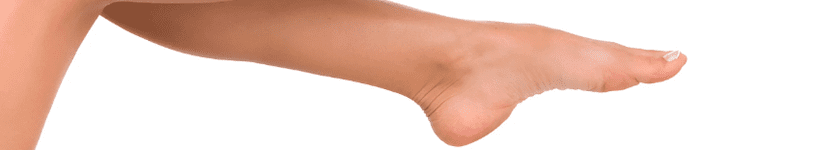
Pes Planus
Flat Feet
What Is Pes Planus?
Pes planus or flat feet is a postural deformity relating to the medial longitudinal arch’s collapse or flattening. As seen in the image, pes planus results in the midfoot region pronating towards the ground and in some cases touching the ground ultimately. Descriptions also include hyperpronation or overpronation. Although there are varying degrees of collapse, people can still live utterly pain-free with flat feet.
What Causes Flat Feet?
This condition can be congenital (e.g., birth) or acquired (e.g. adults, increased exposure to weight-bearing).
Congenital flat feet occur when someone is born with or predisposed to having a more flexible midfoot region resulting in pronation or collapsing of the arch. Ethnicity is a crucial factor surrounding flat feet, which is more likely in certain indigenous cultures.
Acquired flat feet causes include a loss of active (e.g. intrinsic foot and ankle stabilisers) or passive support (ligamentous laxity, hypermobile joints). The lack of support during vigorous weight-bearing activities exaggerates the flatness. Muscular weakness in the ankle and arch stabilisers is the most common etiological factor for flat feet. Research suggests the tibialis posterior muscle is the most integral in stabilising the medial longitudinal arch via its insertion into the arch’s bony roof. When your arch stabilisers perform sub-optimally, the arch slowly pronates and flattens towards the ground when weight and force apply down through the foot.
How Do Flat Feet Progress?
Flat feet slowly progress as you increase your feet’s exposure to weight-bearing activities. The two most common progressions from flat feet are foot deformities and bony stress injuries.
In the active person, hyperpronation alters the load transference up through the leg and can cause stress responses such as shin splints and, in the worst case, stress fractures.
At the opposite end, the bones through your foot are also exposed to altered loads, potentially causing a bunion. As seen in the image, the midfoot pronation and collapse of the arch change the force’s line to the outside of the first metatarsal (from green to red), creating the bony protrusion. As the metatarsal head pushes outwards, the rest of the big toe glides inwards, further accentuating the bunion.
What Conditions Can Flat Feet Cause?
Without an appropriate rehabilitation program and continuing active or passive instability, structures surrounding or supporting the arch can load inappropriately and unsafely to cause compounding problems. The most common compounding problems are listed below:
Tibialis Posterior Tendinopathy
Your tibialis posterior muscle is a vital arch stabiliser. However, if weakness is apparent and the tissue overloads, tendinopathy or muscle injury can occur. More info: Tibialis Posterior Tendinopathy
Plantar Fasciopathy
Better known as plantar fasciitis, plantar fasciopathy can develop due to altered arch biomechanics and increasing midfoot pronation. The plantar fascia is overloaded while compensating for this continuing arch integrity loss.
Medial Tibial Stress Syndrome or “Shin Splints”
The excessive pronation can cause the tibialis posterior or soleus muscle to apply altered stress to the tibia’s inner aspect—this unreasonable motion results in medial tibial stress syndrome: shin splints or tibia stress fractures.
Achilles Tendinopathy
Flat feet can cause the medial aspect of your Achilles tendon to compensate for the increased midfoot motion and exposure to abnormal loads leading to injury. Achilles tendinopathy or its subgroup Achilles tendinitis may be the result.
Patellofemoral Pain Syndrome
Your patella or “kneecap” is commonly affected due to its altered translation during movement. The ankle and knee rotational changes can push the kneecap in the wrong direction, causing anterior knee pain—more info: patellofemoral pain syndrome.
Biomechanical Factors
Excessive or overpronation of the midfoot can cause a cascade effect through the ankle, knee, and hip via inducing tibial and femoral rotation changes and altering these joints’ standard dynamic control. These changes, although sometimes subtle, can predispose your knee and hip joints to increased instability and an increased likelihood of acute trauma.
How are Flat Feet Diagnosed?
The Foot Posture Index (FPI) is an observational tool comprising six items to analyse your static standing posture from 3 different angles. The FPI can assist your physiotherapist in diagnosing flat feet or pes planus. However, your diagnosis should not rely entirely on this one index.
Due to problems most commonly arising in weight-bearing activities, your physiotherapist will observe you conducting numerous single-leg tasks to investigate your overall dynamic control, from your foot and ankle to your hips. Tests will include activities that challenge your strength, endurance, proprioception, and balance. The main focus will be identifying any active insufficiencies through your arch and its’ respective stabilisers.
In some cases, a weight-bearing X-ray may investigate the integrity and dynamic control of the arch’s specific joints under stress and load.
Don’t hesitate to get in touch with your foot physiotherapist for advice specific to your pes planes.
Pes Planus Treatment
Treatment for pes planus can vary, chiefly considering the broad etiological factors. Below is a range of treatment directions focusing primarily on improving the foot and ankle’s active stabilisation to correct the deformity of flat feet.
Restore Intrinsic Muscle Control and Foot Arch Biomechanics
Your foot arch’s important intrinsic plantar muscles, which may be weak or have poor endurance, require retraining. These foot muscles have a vital role in stabilising your foot’s base, preventing overpronation of the midfoot and loading through your plantar fascia.
Dynamic Foot Posture Exercises
Any deficiencies will be an essential component of your rehabilitation. Your physiotherapist can assess and correct your dynamic foot control. They will help restore your normal foot biomechanics and provide foot stabilisation exercises to alleviate deficiencies.
Passive Arch Support / Orthotics
After your biomechanical assessment, a soft temporary orthotic may help provide protection and relief through over-loaded structures. If your physiotherapist deems an orthotic will benefit you long-term, they may refer you to a podiatrist for a custom-made orthotic. The good news is that most flat feet sufferers will not need permanent passive arch support such as an orthotic.
Restore Normal Calf & Leg Muscle Control
You may find it challenging to comprehend, but all of your leg (calf, thigh and hip) muscles are essential in controlling your ankle position and foot arch mechanics. Your physiotherapist will assess your leg muscle function. They’ll provide the necessary treatment or exercises to correct any ankle, knee or hip stabiliser insufficiency. Ask your physiotherapist for more specific advice.
Improve Your Running and Landing Technique
Suppose your flat feet or compounding problems of the ankle or leg exacerbate with sport or running, which place enormous forces through these areas. In that case, a good physiotherapist can analyse your running and landing technique.
Based on that assessment, the treatment you provide will help with technique correction and preventative strategies to reduce the likelihood of injury recurrence.
Return to Sport or Work
Depending on the demands of your chosen sport or job, you may require specific sport-specific or work-specific exercises and a progressed training regime to enable a safe and injury-free return to your chosen sport or employment. While flat feet can be pain-free, for some people, the pain it causes can hamper their working and active life. Specific focus will apply to control your foot arch through particular activities that are causing you discomfort.
Your physiotherapist will discuss your goals, time frames and training schedules with you to optimise your complete and triumphant return to sport or work. Work-related injuries will often require a discussion between your doctor, rehabilitation counsellor or employer.
Footwear Analysis
Sometimes poorly designed footwear can predispose you to acquire flat feet or an associated injury. Suppose you do suffer pain or discomfort that is impacting your active lifestyle. In that case, you should seek the professional advice of your healthcare practitioner to assist your ability in determining the best footwear for your feet.
For more specific advice about your pes planus, please contact your PhysioWorks physiotherapist.
Related Articles
- Bunion Management And Treatment Options: Discusses various foot conditions including bunions, providing insight into their management.
- Anterior Ankle Impingement: Offers a guide on causes, treatments, and tips for anterior ankle impingement, relevant for understanding related ankle issues.
- Ankle Pain: Effective Management And Treatment Options: Explores different causes of ankle pain and provides treatment options, emphasizing the importance of addressing biomechanical issues like flat feet.
- Heel Pain: Investigates causes of heel pain, linking conditions such as plantar fasciitis and heel spurs to flat feet, thus offering a comprehensive look at foot pain sources.
- Plantar Fasciitis: Specifically targets plantar fasciitis, detailing its relationship with flat feet and providing insights into treatment and prevention.
- Metatarsalgia: Examines the pain in the ball of the foot, known as metatarsalgia, discussing how foot biomechanics, including flat feet, can influence such conditions.
- Foot Pain: Provides an overview of common sources of foot pain, including biomechanical conditions like flat feet, and suggests possible treatments.
Common Foot Pain Causes


Various factors, ranging from injuries and tendon problems to degenerative conditions and systemic diseases, can cause foot pain. Some common causes of foot pain include foot injuries, plantar fasciitis, bunions, metatarsalgia, Morton's neuroma, tendon injuries, bone injuries, degenerative conditions like arthritis, biomechanical issues, nerve-related sources such as tarsal tunnel syndrome, and muscle injuries.
Certain systemic conditions like fibromyalgia, lupus, rheumatoid arthritis, and psoriatic arthritis can also contribute to foot pain. This comprehensive list covers a wide range of foot pain causes, encompassing different areas of the foot and various underlying conditions.
Foot Injuries
Tendon Injuries
- Achilles Tendon Rupture
- Achilles Tendinopathy
- FHL Tendinopathy
- Peroneal Tendinopathy
- Tibialis Posterior Tendinopathy
Bone Injuries
- Ankle Fracture (Broken Ankle)
- Stress Fracture
- Stress Fracture Feet
- Severs Disease
- Osteochondritis Dissecans
- Heel Spur
- Shin Splints
Traumatic Ankle Ligament Injuries
Degenerative Conditions
Soft Tissue Inflammation
Biomechanical Conditions
Nerve-Related Sources
Muscle Injuries
Systemic Conditions
Soft Tissue Inflammation
Other Useful Information
Foot, Ankle & Heel Pain FAQs
Introduction
Welcome to PhysioWorks' comprehensive FAQ page on Foot, Ankle, and Heel Pain. Our expert physiotherapists are here to guide you in managing and overcoming discomfort. We’ve organised the FAQs into categories, each with a brief overview and links to in-depth articles, making navigation and understanding easier for you.


Foot Pain
Step into the various causes of foot pain and learn effective ways to relieve discomfort. Understand the impact of activities like barefoot running.
Ankle Injuries
Explore common ankle injuries and how to address them. From sprains to ligament damage, find out the best practices for care and prevention.
Heel Pain
Uncover the reasons behind heel pain and the effective treatments available. This section is particularly useful for understanding conditions like plantar fasciitis and heel spurs.
Achilles Pain
Find out how to manage and treat Achilles tendinopathy, a common concern for athletes and active individuals.
Shin Pain
Learn about shin splints, their causes, and how to alleviate this common issue, especially among runners.
Youth Injuries
Gain insights into youth leg injuries, including growing pains and heel issues in children.
Balance & Proprioception
Enhance your balance and proprioception with our professional advice and exercises.
Related Articles
- Sprained Ankle Treatment & Recovery Guide: Offers detailed advice on how to manage sprained ankles, including immediate recovery steps and physiotherapy treatments.
- Ankle Pain: Effective Management And Treatment Options: Discusses various conditions leading to ankle pain and outlines effective treatment strategies, highlighting the role of physiotherapy in pain reduction and mobility improvement.
- Plantar Fasciitis: Provides an overview of plantar fasciitis, including common causes, treatment options, and related conditions like peroneal tendinopathy and Achilles tendinopathy.
- Achilles Tendinopathy: Focuses on the causes of Achilles tendinopathy, its impact on heel pain, and a range of treatment and prevention strategies.
- Ankle Strapping: Complete Guide To Injury Prevention: Explains the benefits of ankle strapping as a preventative measure against injuries, with a focus on techniques and materials.
- Heel Pain: Explores various causes of heel pain, including tendon injuries, foot injuries, bone injuries, and systemic conditions, alongside recommended treatments.