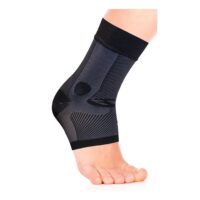
Posterior Ankle Impingement
Article by Zoe Russell
Posterior Ankle Impingement: Comprehensive Treatment and Prevention Guide
What is Posterior Ankle Impingement?
Posterior Ankle Impingement is a condition where pain is experienced at the back of the ankle due to compression of bone or soft tissue structures during activities that involve maximal ankle bending downwards (plantarflexion motion). This condition is also known by several other names, such as Ankle Impingement, Posterior Impingement Syndrome, Posterior Impingement of the Ankle, or Os Trigonum Syndrome.
The Ankle’s Anatomy and Impingement Mechanics
The ankle joint comprises the tibia and talus, which glide on one another, cushioned by articular cartilage. This cartilage helps absorb the impact of the tibia on the talus during weight-bearing activities. During plantar flexion, where the foot and ankle point maximally away from the body, the ankle experiences compression. This compression may cause tissue damage and pain, especially if the forces are repetitive or excessively forceful.

Who is at Risk?
Posterior ankle impingement commonly affects athletes such as gymnasts, ballet dancers, footballers, and cricket fast bowlers (especially the front or landing leg). Inadequate rehabilitation following an acute ankle injury often leads to this condition. Some individuals may have an anatomical variant in their talus bone, known as an os trigonum, which increases the likelihood of developing this condition, particularly in active individuals.
Symptoms of Posterior Ankle Impingement
The typical presentation includes sharp pain at the back of the ankle, particularly during activities requiring maximal plantar flexion. An ache may persist at rest or after provocative activities like kicking a ball, dancing on pointe, running downhill, jumping, or activities performed on tippy-toes.
Diagnosis and Imaging Techniques
Diagnosis includes an assessment of your history and a physical examination by your physiotherapist. Imaging, such as standard ankle radiographs (X-rays) or Magnetic Resonance Imaging (MRI), might be recommended to confirm the diagnosis. MRIs are particularly useful as they can rule out other causes of foot or ankle pain and show signs of swelling in the affected area, assisting in surgical planning if necessary.
Ankle Impingement Treatment Guidelines
Phase I: Managing Pain and Swelling
Pain management is crucial in the initial treatment. This includes active rest (avoiding activities that provoke pain), applying ice, compression, and elevating the ankle to reduce swelling. Your physiotherapist may use various treatments, such as electrotherapy, acupuncture, or taping techniques, to reduce pain and inflammation. In some cases, anti-inflammatory medication and natural creams like arnica can also be beneficial.
Phase 2 and 3: Restoring Motion and Strength
It’s important to regain full motion in your ankle as soon as it’s comfortable. This is followed by exercises to strengthen your calf, ankle, and foot muscles, essential for recovery and prevention of future injuries.
Phase 4: Enhancing Speed and Agility
Particularly for athletes, it’s vital to restore balance, speed, and agility to safely return to high-speed activities. Tailored exercises will help achieve this.
Phase 5: Returning to Normal Activities
The final phase involves returning to daily activities and sports. Your physiotherapist will customize your training schedule, ensuring a safe return and minimizing the risk of re-injury.
When Surgery is an Option
Surgery is considered for persistent cases, particularly for high-level athletes. It involves removing bone spurs or soft tissue that cause impingement. However, surgery won’t be helpful if the pain is due to significant ankle arthritis.
Other Treatment Options
Treatments like corticosteroid injections or acupuncture can provide relief, alongside maintaining general fitness through appropriate exercises.
Conclusion
Posterior Ankle Impingement requires careful and professional management. With appropriate physiotherapy and, in some cases, surgery, pain can be alleviated, and a return to normal activities can be achieved.
What to Do?
Consult a physiotherapist if you suspect Posterior Ankle Impingement. They will provide specific advice and guide you through the recovery process.
Related Articles
Common Causes of Ankle Pain
Introduction
Welcome to our detailed guide on the common causes of ankle pain. As physiotherapists, we understand how various conditions and injuries can lead to discomfort in your ankle. From sprains to degenerative diseases, this guide aims to provide clear insights for the general public on navigating these issues.


Sprained Ankles and Syndesmosis Injuries
Sprained ankles, including syndesmosis injuries, are among the most common issues we encounter. These injuries can range from mild ligament stretches to severe tears, impacting your mobility and quality of life. Understanding the specifics of each type is crucial for effective treatment and timely recovery.
Ankle Tendinopathies
Tendinopathies, such as those affecting the Achilles and tibialis posterior tendons, are common in active individuals. These conditions arise due to overuse or trauma, leading to pain and swelling in the affected area. Targeted physiotherapy can significantly aid in recovery and prevent future injuries.
Posterior Ankle Conditions
Conditions like posterior ankle impingement and retrocalcaneal bursitis can cause significant pain, especially during physical activities. Recognising these conditions early and starting appropriate treatment is vital for maintaining ankle health and functionality.
Ankle Arthritis
Arthritis in the ankle, often a result of wear and tear or injury, leads to joint pain and stiffness. Early intervention and proper management, including physiotherapy, are essential to slow its progression and manage symptoms effectively.
Biomechanical Conditions
Abnormal foot and ankle biomechanics can lead to various issues, from pain during weight-bearing to nerve compression. Understanding and treating these conditions are crucial for restoring normal function and preventing further complications.
Systemic Conditions That May Cause Ankle Pain
Systemic diseases such as rheumatoid arthritis can manifest as ankle pain. It's important to address these underlying conditions to effectively manage ankle symptoms.
Conclusion
Ankle pain can arise from a multitude of causes, each requiring a unique approach to treatment. If you're experiencing ankle discomfort, we recommend consulting a physiotherapist or doctor for a thorough evaluation. A personalised care plan can significantly improve your quality of life and mobility.
Related Articles
- Sprained Ankle Treatment & Recovery Guide - This article provides comprehensive information on managing pain and inflammation for a sprained ankle, including initial RICE steps and exercises for restoring mobility.
- Anterior Ankle Impingement: Causes, Treatments, Tips & Guide - Offers insights into the causes of anterior ankle impingement, its treatments, and practical tips for management.
- Posterior Ankle Impingement: Causes & Treatments - Explains the condition of posterior ankle impingement, its causes, and available treatment options.
- Tibialis Posterior Tendinopathy - Discusses the condition affecting the tibialis posterior tendon, symptoms, and implications for foot arch pain and ankle stability.
- Achilles Tendinopathy - Answers frequently asked questions about foot and ankle pain associated with Achilles tendinopathy and provides an overview of tendon injuries.
- How To Strap An Ankle - Guides on the correct techniques and types of tape for ankle strapping to prevent or manage ankle injuries.
Foot, Ankle & Heel Pain FAQs
Introduction
Welcome to PhysioWorks' comprehensive FAQ page on Foot, Ankle, and Heel Pain. Our expert physiotherapists are here to guide you in managing and overcoming discomfort. We’ve organised the FAQs into categories, each with a brief overview and links to in-depth articles, making navigation and understanding easier for you.


Foot Pain
Step into the various causes of foot pain and learn effective ways to relieve discomfort. Understand the impact of activities like barefoot running.
Ankle Injuries
Explore common ankle injuries and how to address them. From sprains to ligament damage, find out the best practices for care and prevention.
Heel Pain
Uncover the reasons behind heel pain and the effective treatments available. This section is particularly useful for understanding conditions like plantar fasciitis and heel spurs.
Achilles Pain
Find out how to manage and treat Achilles tendinopathy, a common concern for athletes and active individuals.
Shin Pain
Learn about shin splints, their causes, and how to alleviate this common issue, especially among runners.
Youth Injuries
Gain insights into youth leg injuries, including growing pains and heel issues in children.
Balance & Proprioception
Enhance your balance and proprioception with our professional advice and exercises.
Related Articles
- Sprained Ankle Treatment & Recovery Guide: Offers detailed advice on how to manage sprained ankles, including immediate recovery steps and physiotherapy treatments.
- Ankle Pain: Effective Management And Treatment Options: Discusses various conditions leading to ankle pain and outlines effective treatment strategies, highlighting the role of physiotherapy in pain reduction and mobility improvement.
- Plantar Fasciitis: Provides an overview of plantar fasciitis, including common causes, treatment options, and related conditions like peroneal tendinopathy and Achilles tendinopathy.
- Achilles Tendinopathy: Focuses on the causes of Achilles tendinopathy, its impact on heel pain, and a range of treatment and prevention strategies.
- Ankle Strapping: Complete Guide To Injury Prevention: Explains the benefits of ankle strapping as a preventative measure against injuries, with a focus on techniques and materials.
- Heel Pain: Explores various causes of heel pain, including tendon injuries, foot injuries, bone injuries, and systemic conditions, alongside recommended treatments.