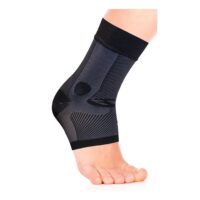
Peroneal Tendinopathy
Article by John Miller
What is Peroneal Tendinopathy?
Peroneal tendinopathy refers to a condition where the peroneal tendon undergoes structural changes in response to excessive loading, which can result from overuse or other factors. Although people often use the term “peroneal tendonitis” interchangeably with peroneal tendinopathy, it can be misleading since inflammation is not always the primary feature of this condition. Instead, the tendon may become irritated and swollen due to the mechanical stresses placed on it, but without significant inflammatory response.
The term tendinopathy describes any disorder related to tendons that involves changes in the structure, composition, and mechanical properties of the tendon.In the case of peroneal tendinopathy, the tendon may thicken, degenerate, or develop small tears or nodules. These changes can lead to pain, weakness, stiffness, and instability of the ankle and foot, which can affect daily activities and sports performance.
If you suspect you have peroneal tendinopathy, it is important to seek medical advice from a qualified healthcare professional, such as a sports medicine physician, physiotherapist, or orthopaedic surgeon, who can provide an accurate diagnosis and appropriate treatment plan based on your specific condition and needs.
What are the Peroneal Muscles?
The peroneal muscles, also known as the fibular muscles, are a group of muscles located on the lateral side of the lower leg. They consist of the peroneus longus and peroneus brevis muscles, which originate from the fibula bone and run down to the foot, where they insert into various bones and joints.
The peroneal muscles are responsible for several important functions related to foot and ankle movement and stability. They help to turn the foot outward (eversion), which is essential for walking and running on uneven surfaces. They also provide lateral support to the ankle joint, helping to prevent ankle sprains and other injuries during weight-bearing activities.
The peroneal tendons are two thick fibrous cords that wrap around the lateral malleolus, the bony prominence on the outer side of the ankle, and attach to the bones and muscles of the foot. These tendons are constantly under tension whenever the peroneal muscles contract to control foot and ankle movements.
What Causes Peroneal Tendinopathy?
Peroneal tendinopathy is a condition that can develop gradually over time or occur suddenly due to various factors that affect the peroneal tendons and muscles. Some of the most common causes of peroneal tendinopathy include:
- Overuse or excessive loading: Activities that involve repetitive or prolonged weight-bearing on the foot and ankle, such as running, jumping, or cutting sports, can strain the peroneal tendons and lead to microtears, degeneration, or thickening of the tendon.
- Poor footwear or foot mechanics: Wearing shoes that do not fit properly or provide enough support, or having abnormal foot and ankle mechanics, such as flat feet, high arches, or ankle instability, can increase the stress on the peroneal tendons and muscles and make them more susceptible to injury.
- Muscle imbalances and weaknesses: Imbalances in the strength and flexibility of the lower leg muscles, particularly the peroneals, gastrocnemius, and soleus, can alter the way the foot and ankle move and distribute forces, leading to abnormal stress on the peroneal tendons.
- Previous ankle injuries: A history of ankle sprains, fractures, or other injuries can weaken the peroneal tendons and make them more prone to damage during subsequent activities.
- Other factors: Certain medical conditions, such as rheumatoid arthritis, gout, or diabetes, can affect the health of the tendons and increase the risk of peroneal tendinopathy.
What are the Symptoms of Peroneal Tendinopathy?
Peroneal tendinopathy is a condition that affects the tendons located on the outside of the ankle. The following are some of the common symptoms associated with this condition:
- Gradual worsening of pain on the outer part of the ankle
- Pain during or after weight-bearing activities, such as walking or running
- Pain when turning the foot inward or outward
- Ankle instability when bearing weight
If you experience any of these symptoms, it’s important to consult a medical professional for an accurate diagnosis and appropriate treatment.
How is Peroneal Tendinopathy Diagnosed?
Qualified healthcare professionals, such as physiotherapists or doctors, typically diagnose peroneal tendinopathy. They may conduct a series of tests to assess the affected area and rule out other potential causes of lateral ankle pain.
Along with physical tests, an ultrasound scan can confirm the diagnosis of peroneal tendinopathy. This non-invasive imaging test provides a detailed view of the tendons and surrounding tissues, ensuring a more accurate diagnosis.
If you’re experiencing symptoms of peroneal tendinopathy, it’s crucial to seek medical attention promptly. Timely and accurate diagnosis is essential to receive the appropriate treatment and prevent the condition from worsening.
Peroneal Tendinopathy Treatment
The treatment of peroneal tendinopathy depends on the severity and stage of the injury. In general, the earlier the condition is detected and treated, the better the prognosis.
During the acute phase, the focus of treatment is to reduce the load on the affected tendon and allow it to heal. This may include rest, ice, compression, and elevation (RICE), as well as the use of a brace or orthotic device to support the ankle. Once the pain subsides, a home exercise program may be prescribed to improve range of motion, strengthen the lower limb muscles, and enhance balance.
Chronic peroneal tendinopathies may take longer to recover, and the treatment approach is focused on active rehabilitation to improve the tendon’s ability to respond to load. This may include eccentric strengthening exercises for the peroneal muscles and lower limb, as well as exercises to improve balance, strength, and range of motion. In some cases, surgery may be required to repair or remove damaged tendon tissue.
It’s important to work with a qualified healthcare professional, such as a physiotherapist or doctor, to develop an individualised treatment plan that meets your specific needs and goals. Consistent adherence to the treatment plan and proper rehabilitation can help you recover from peroneal tendinopathy and prevent future injury.
Peroneal Tendinopathy Prevention
Peroneal tendinopathy can be a painful and debilitating condition, but there are steps you can take to prevent it from developing. Here are some tips for reducing your risk of peroneal tendinopathy:
- Wear supportive footwear that fits correctly, and is appropriate for your chosen activity. This doesn’t necessarily mean the most expensive or latest shoe on the market, but rather one that provides adequate support and cushioning for your foot type and activity level.
- Gradually increase your training load or exercise level. Sudden increases in activity can put stress on the tendons and increase the risk of injury. Increase your intensity, duration, or frequency of exercise slowly and incrementally over time.
- Maintain a level of activity in the “off-season” through cross-training or other low-impact activities. This can help you maintain your cardiovascular fitness and keep your muscles healthy, reducing your risk of re-injury when you return to your primary sport or activity.
- Improve your balance and ankle proprioception through exercises like single-leg balance drills, agility drills, or wobble board exercises. This can help improve the strength and stability of the ankle joint, reducing the risk of injury.
By incorporating these preventive measures into your routine, you can help reduce your risk of developing peroneal tendinopathy and enjoy a safe and healthy active lifestyle.
Return to Sports with Peroneal Tendinopathy
For athletes with peroneal tendinopathy, the goal of treatment is to manage pain and inflammation, restore normal function, and prevent further injury. With proper treatment and rehabilitation, most people are able to return to their previous level of sporting activity without any ongoing problems.
It’s important to note, however, that the recovery process can be lengthy and requires patience and commitment. You must follow your rehabilitation program as prescribed by your physiotherapist, as well as modifications to your training routine.
Returning to sports too soon or without completing your rehabilitation program increases the risk of re-injury, which can lead to chronic problems and longer recovery times. It’s important to seek professional treatment and guidance to ensure a safe and successful return to sports.
If you are experiencing symptoms of peroneal tendinopathy or any other musculoskeletal injury, seek the advice of a qualified healthcare professional, such as a physiotherapist or doctor. They can provide a proper diagnosis, develop an individualised treatment plan, and guide you through the rehabilitation process to help you return to your active lifestyle.
Tendinopathy FAQs
Common Causes of Ankle Pain
Introduction
Welcome to our detailed guide on the common causes of ankle pain. As physiotherapists, we understand how various conditions and injuries can lead to discomfort in your ankle. From sprains to degenerative diseases, this guide aims to provide clear insights for the general public on navigating these issues.


Sprained Ankles and Syndesmosis Injuries
Sprained ankles, including syndesmosis injuries, are among the most common issues we encounter. These injuries can range from mild ligament stretches to severe tears, impacting your mobility and quality of life. Understanding the specifics of each type is crucial for effective treatment and timely recovery.
Ankle Tendinopathies
Tendinopathies, such as those affecting the Achilles and tibialis posterior tendons, are common in active individuals. These conditions arise due to overuse or trauma, leading to pain and swelling in the affected area. Targeted physiotherapy can significantly aid in recovery and prevent future injuries.
Posterior Ankle Conditions
Conditions like posterior ankle impingement and retrocalcaneal bursitis can cause significant pain, especially during physical activities. Recognising these conditions early and starting appropriate treatment is vital for maintaining ankle health and functionality.
Ankle Arthritis
Arthritis in the ankle, often a result of wear and tear or injury, leads to joint pain and stiffness. Early intervention and proper management, including physiotherapy, are essential to slow its progression and manage symptoms effectively.
Biomechanical Conditions
Abnormal foot and ankle biomechanics can lead to various issues, from pain during weight-bearing to nerve compression. Understanding and treating these conditions are crucial for restoring normal function and preventing further complications.
Systemic Conditions That May Cause Ankle Pain
Systemic diseases such as rheumatoid arthritis can manifest as ankle pain. It's important to address these underlying conditions to effectively manage ankle symptoms.
Conclusion
Ankle pain can arise from a multitude of causes, each requiring a unique approach to treatment. If you're experiencing ankle discomfort, we recommend consulting a physiotherapist or doctor for a thorough evaluation. A personalised care plan can significantly improve your quality of life and mobility.
Related Articles
- Sprained Ankle Treatment & Recovery Guide - This article provides comprehensive information on managing pain and inflammation for a sprained ankle, including initial RICE steps and exercises for restoring mobility.
- Anterior Ankle Impingement: Causes, Treatments, Tips & Guide - Offers insights into the causes of anterior ankle impingement, its treatments, and practical tips for management.
- Posterior Ankle Impingement: Causes & Treatments - Explains the condition of posterior ankle impingement, its causes, and available treatment options.
- Tibialis Posterior Tendinopathy - Discusses the condition affecting the tibialis posterior tendon, symptoms, and implications for foot arch pain and ankle stability.
- Achilles Tendinopathy - Answers frequently asked questions about foot and ankle pain associated with Achilles tendinopathy and provides an overview of tendon injuries.
- How To Strap An Ankle - Guides on the correct techniques and types of tape for ankle strapping to prevent or manage ankle injuries.
Foot, Ankle & Heel Pain FAQs
Introduction
Welcome to PhysioWorks' comprehensive FAQ page on Foot, Ankle, and Heel Pain. Our expert physiotherapists are here to guide you in managing and overcoming discomfort. We’ve organised the FAQs into categories, each with a brief overview and links to in-depth articles, making navigation and understanding easier for you.


Foot Pain
Step into the various causes of foot pain and learn effective ways to relieve discomfort. Understand the impact of activities like barefoot running.
Ankle Injuries
Explore common ankle injuries and how to address them. From sprains to ligament damage, find out the best practices for care and prevention.
Heel Pain
Uncover the reasons behind heel pain and the effective treatments available. This section is particularly useful for understanding conditions like plantar fasciitis and heel spurs.
Achilles Pain
Find out how to manage and treat Achilles tendinopathy, a common concern for athletes and active individuals.
Shin Pain
Learn about shin splints, their causes, and how to alleviate this common issue, especially among runners.
Youth Injuries
Gain insights into youth leg injuries, including growing pains and heel issues in children.
Balance & Proprioception
Enhance your balance and proprioception with our professional advice and exercises.
Related Articles
- Sprained Ankle Treatment & Recovery Guide: Offers detailed advice on how to manage sprained ankles, including immediate recovery steps and physiotherapy treatments.
- Ankle Pain: Effective Management And Treatment Options: Discusses various conditions leading to ankle pain and outlines effective treatment strategies, highlighting the role of physiotherapy in pain reduction and mobility improvement.
- Plantar Fasciitis: Provides an overview of plantar fasciitis, including common causes, treatment options, and related conditions like peroneal tendinopathy and Achilles tendinopathy.
- Achilles Tendinopathy: Focuses on the causes of Achilles tendinopathy, its impact on heel pain, and a range of treatment and prevention strategies.
- Ankle Strapping: Complete Guide To Injury Prevention: Explains the benefits of ankle strapping as a preventative measure against injuries, with a focus on techniques and materials.
- Heel Pain: Explores various causes of heel pain, including tendon injuries, foot injuries, bone injuries, and systemic conditions, alongside recommended treatments.