Spondylolysis
Article by John Miller
Spondylolysis
Understanding Stress Fractures in the Back
Spondylolysis Explained
Spondylolysis describes a stress fracture affecting the pars interarticularis of the spine. This fracture commonly leads to structural back pain among children, adolescents, and active adults, particularly at the L5 vertebral level, with a prevalence of 90-95%.
This condition presents in various forms: dysplasic, isthmic (from sports), degenerative, or traumatic, with the isthmic type being predominant. Spondylolysis can cause spondylolisthesis, which is a slippage of the vertebral body seen in roughly half of the cases, especially when spondylolysis is bilateral, or there’s mechanical instability, often observed in females. Notably, some nonunion fractures form a fibrous mesh rather than bone, although complete healing of the stress lesion is typical.
Symptoms of Spondylolysis
Patients typically report unilateral back pain which intensifies with activities like arching or standing that stress the pars interarticularis. While the initial pain may be sharp, it dulls over time and often eases with rest. Approximately 80% of sufferers exhibit a pronounced back arch and tight hamstrings.
Causes and Age of Onset
Activities that excessively bend or twist the spine, such as certain sports, can cause spondylolysis. It can emerge in early childhood or adolescence, with a higher incidence in males.
Diagnosing Spondylolysis
Diagnostic scans, including oblique X-rays, bone scintigraphy, CT, MRI, and SPECT bone scans, are vital for detecting spondylolysis. These scans are complemented by physical exams that typically reveal back pain and hamstring tightness without neurological symptoms.
High-Risk Sports for Back Stress Fractures

Identifying Risky Activities
Certain sports exert significant stress on the spine, increasing the risk of spondylolysis. Activities that involve repetitive twisting, hyperextension, or impact can predispose athletes to stress fractures in the back.
Sports with Elevated Risks
Cricket: Bowlers in cricket often engage in repetitive, fast-twisting motions during delivery, placing them at a higher risk.
Gymnastics: The sport requires extreme spinal flexion and extension, making gymnasts particularly susceptible.
Weightlifting: Lifters experience high spinal loads during squats and deadlifts, which can lead to stress fractures.
Wrestling and Judo: These combat sports involve forceful twisting and hyperextension movements.
Swimming: Butterfly strokes specifically can stress the lower back through repetitive arching motions.
Ballet and Dance: Dancers often perform hyperextensions as part of their routines.
Ice Skating: Skaters are at risk due to jumps and landings that jar the spine and the need for strong back arches in some movements.
Track and Field: Events like javelin throwing involve sudden hyperextensions and rotations of the spine.
Golf: Golfers risk stress fractures due to the rotational force exerted on the spine during swings.
Diving: Divers repeatedly arch their backs with significant force when entering the water.
American Football: The impact and physical nature of football, along with the arching stances, contribute to spinal stress.
Minimising Risks in High-Impact Sports
Athletes participating in these sports should take preventive measures, such as engaging in core-strengthening exercises, maintaining flexibility, and ensuring proper technique. Coaches and healthcare providers should monitor athletes for signs of overuse and encourage appropriate rest and recovery periods.
Understanding these risks empowers athletes to seek early intervention if symptoms arise, facilitating a quicker return to their passion with a stronger, healthier back.
Treating Spondylolysis
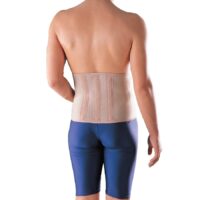
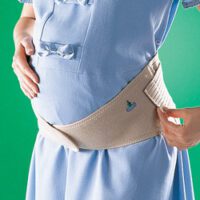
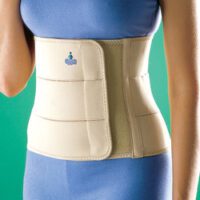
The first line of treatment for spondylolysis centres on alleviating pain and promoting healing. Resting from activities that aggravate the condition is essential. The strategic use of a back brace serves to manage discomfort and safeguard the injury site during recovery. The importance of conservative treatment is paramount, as bilateral fractures of the pars interarticularis can lead to persistent instability and lifelong spinal alterations. The expert guidance of a spinal physiotherapist, who understands the demands of your sport, is crucial to avert the progression to more invasive interventions, such as spinal surgery, or the cessation of sporting activities altogether.
Rehabilitation and Prevention
Rehabilitation aims to restore joint mobility, increase muscle flexibility, and build strength. Physiotherapist-guided exercises are often the cornerstone of this process, with Pilates playing a key role in the latter stages of rehabilitation and prevention. The goal is to reinforce the back and core muscles to dynamically support and protect the lower back from further stress.
When to Consider Surgery
Surgery should be considered a last resort, recommended only after all conservative treatments have been exhausted without providing relief from severe, ongoing symptoms. Carefully evaluating the potential risks and benefits with healthcare professionals is essential before opting for spinal surgery.
Prognosis
The recovery period for most individuals with spondylolysis extends up to 3 or 4 months, although athletes engaged in high-risk sports may require a longer rehabilitation period. While non-surgical treatments are often successful, the risk of re-injury remains if the factors contributing to the initial injury are not fully addressed.
Conclusion
In sum, spondylolysis is a prevalent spinal condition, especially among young, athletic populations. Early recognition and management are key to overcoming this condition. Conservative treatment strategies, focusing on pain relief and muscle strengthening, are effective for most, facilitating a return to everyday activities and sports. Nevertheless, preventive measures must continue beyond the disappearance of symptoms to prevent recurrence and maintain spinal integrity. For persistent cases that challenge conservative management, surgery may be necessary, but this requires judicious deliberation.
Ultimately, a customised treatment plan, devised by experienced medical professionals, ensures the best possible outcome, allowing individuals to enjoy an active lifestyle without the hindrance of back pain.
Related Articles
- Back Pain Physiotherapy: Your Guide to What to Expect: Offers insights into physiotherapy approaches for back pain, including conditions like Spondylolysis.
- Spondylolisthesis: Explores Spondylolisthesis, a condition often linked with Spondylolysis, involving vertebra displacement.
- Core Stability: A Physiotherapist’s Guide for Spinal Health: Discusses core stability’s importance for spinal health, crucial in managing Spondylolysis.
- Cricket Back Stress Fractures: Focuses on cricket, a sport with high incidence of back stress fractures, relevant to Spondylolysis.
- Swimmers Back: Essential Guide to Lower Back Pain: Provides prevention and management tips for back issues in swimmers, including Spondylolysis.
- Stress Fracture Management and Prevention – Physio Guide: Emphasises physiotherapy in recovery and prevention of stress fractures, including those in the back seen in Spondylolysis.
What Causes Lower Back Pain?
Introduction
Lower back pain is a widespread issue in Australia, stemming from diverse conditions. As physiotherapists, we often encounter various causes of this pain. This guide aims to shed light on these causes and provide valuable insights for effective management.


Muscle-Related Injuries
Muscle injuries are a predominant cause of lower back pain, including:
- Back Cramps and Muscle Pain: Typically resulting from overuse or strain.
- Core Stability Deficiency: Weak core muscles can lead to increased back strain.
- DOMS (Delayed Onset Muscle Soreness): Soreness affecting back muscles post-exercise.
Recent research underscores the importance of regular exercise and core strengthening in preventing these injuries.
Bone-Related Injuries
Bone health is crucial in lower back pain, encompassing conditions like:
- Spondylosis: Degenerative spine conditions.
- Spondylolysis or Stress Fracture: Common in athletes, such as cricket bowlers.
- Spondylolisthesis: Occurs when a vertebra slips over another.
- Osteoporosis: Causes bones to weaken, increasing fracture risk. Advancements in bone density scanning have improved early detection and management.
- Scheuermann’s Disease: Affects spinal bone growth in teenagers.
- Scoliosis: An abnormal curvature of the spine causing pain.
- Spinal Stenosis: A narrowing of the spinal canal leading to nerve compression.
Disc-Related Injuries
Spinal discs are vital for spinal health:
- Bulging and Disc Protrusions: These discs protrude or "slip" and can press on nerves.
- Herniated Disc: A more severe form of disc protrusion.
- Degenerative Disc Disease: Age-related disc wear and tear.
Minimally invasive surgical techniques have transformed the treatment of severe disc-related injuries where physiotherapy and other non-operative options fail to improve.
Back Joint Injuries
- Facet Joint Pain: Arises from arthritis or stress on these spinal joints.
Nerve-Related Injuries
Nerve issues can lead to:
- Nerve Pain and Pinched Nerves: Caused by spinal nerve compression from disc bulging or arthritic changes.
- Sciatica: Irritation of the sciatic nerve.
Physiotherapy and newer medications have been effective in managing these conditions. Some will require injection therapies or surgery.
Pelvis-Related Injuries
Pelvic issues also contribute to lower back pain:
- Sacroiliac Joint Pain: Involving joints connecting the spine to the pelvis.
- Piriformis Syndrome: Where the piriformis muscle irritates the sciatic nerve.
Pregnancy-Related Pain
- Pregnancy Back Pain: Often due to increased back strain during pregnancy. Prenatal physiotherapy programs are beneficial.
Systemic Diseases
Systemic diseases like Ankylosing Spondylitis, Fibromyalgia and Rheumatoid Arthritis can cause back pain.
Recent Research and Advancements
Current research emphasises a holistic approach to treating lower back pain. Techniques like yoga and Pilates, alongside traditional physiotherapy, and conservatively progressed gym programs show significant relief. The role of diet in managing weight and inflammation is increasingly recognised.
Best Treatments for Lower Back Pain
Treatment varies but often includes:
- Physiotherapy
- Pain management
- Strength and flexibility exercise programs
- Ergonomic adjustments
- Surgical interventions for severe cases
Conclusion
Lower back pain is a significant health concern in Australia. Understanding its causes and seeking professional physiotherapy advice can greatly improve life quality. Remember, early intervention is key for an effective recovery.
What to Do?
If you're experiencing lower back pain, it's vital to consult a physiotherapist or doctor. They can provide an assessment and customised treatment plan based on your specific condition.
Back Pain FAQs & Products
Your Comprehensive Guide to FAQs, Causes, and Relief
Experiencing back pain and looking for answers? Our comprehensive FAQ section covers everything you need to know about back pain - from common causes and symptoms to effective treatments.
Click the links to our detailed articles to understand better and manage your back pain. Explore links to related topics like 'Severe Back Pain Management', 'Posture Improvement Techniques', and 'Physiotherapy for Chronic Back Issues' for a holistic approach to your spinal health."


What Causes Back Pain?
Discover the various factors behind back pain, including muscle strains, herniated discs, and more.
- Most Common Causes of Back Pain
- Causes of Lower Back Pain
- Causes of Upper Back Pain
- Understanding Herniated Discs
- Osteoarthritis and Back Pain
- Back Stress Fractures
- Pregnancy Back Pain
How Can I Relieve Back Pain?
Explore treatments ranging from physiotherapy to exercises, tailored to alleviate back pain.
- Best Treatment for Lower Back Pain
- Physiotherapy for Back Pain
- Exercises for Back Strength
- Could Ultrasound Physiotherapy Help You Beat Back Pain?
- Benefits of Back Massage
Can Back Pain Be Prevented?
Learn how to prevent back pain through healthy habits and proper body mechanics.
- Preventing Back Pain Tips
- Proper Back Posture Guidelines
- Regular Exercise Routines for Back Pain
- Gym Back Exercises
When Should You See a Physio or Doctor for Back Pain?
Understand when it's crucial to seek professional medical advice for back pain.
- Severe Back Pain? Causes, Symptoms & Treatment
- Warning Signs of Severe Back Conditions
- Physiotherapy Consultation for Back Pain: What to Expect?
Repeated Bouts & Incidental Back Pain FAQs
Addressing frequently occurring and sudden back pain incidents.
- Causes of Recurrent Back Strains
- Understanding Sudden Back Pain
- What Causes Back Pain for No Reason?
- What Causes Repeat Low Back Strains & Sprains?
Youth Back Pain FAQs
Focusing on the prevention and management of back pain in teenagers.
Back Pain Exercises FAQs
Discover effective exercises and tools for back pain relief.
- Core Strengthening Exercises
- Exercise Balls for Lower Back Pain and Core Stability
- Is Walking Good for Back Pain?
- Pilates for Back Pain
Back Pain Prevention FAQs
Key insights into everyday activities and their impact on back health.
- Walking and Back Pain
- Handling Recurring Back Pain
- Healthy Weight Maintenance for Back Pain
Posture FAQs
Learn about the importance of good posture and techniques to improve it.
- Importance of Good Posture
- Correct Sitting Posture
- Improving Standing Posture
- Healthy Sleeping Postures
Other Treatments For Back Pain?
Investigate a variety of treatments, from nerve blocks to spinal cord stimulation.
- Epidural Steroid Injections
- Nerve Blocks for Pain Relief
- Spinal Cord Stimulation
- Surgical Options: When to Consider Surgery?
Conclusion
Empowering you with knowledge to understand, address, and prevent back pain effectively.
What to Do Next
Now that you've gained insight into the causes and remedies of back pain, it's time to take the next steps. Start by applying the prevention techniques and exercises detailed in this guide to your daily routine. If you're currently experiencing back pain, consider the treatment options discussed and consult a healthcare professional for personalised advice. Remember, every journey to back health is unique.
Stay informed, be proactive in your self-care, and don't hesitate to seek professional help when needed. For further reading, explore the hyperlinked articles to deepen your understanding and support your path to a pain-free life. Here’s to taking control of your back health and embracing a more comfortable, active lifestyle.