Scoliosis
Article by John Miller
Scoliosis
Understanding and Managing Spinal Curvature
Scoliosis, a condition marked by an abnormal curvature of the spine, creates an “S” or “C” shape rather than a straight line. About 2% of people are affected, with 10% of cases being severe. The curvature’s peak, or apex, usually occurs in the mid-back or where the thoracic and lumbar regions meet, seldom affecting the neck.
The Importance of Early Diagnosis in Scoliosis
Identifying scoliosis early, particularly between ages 11 and 14, is vital to halt its progression into adulthood. Early action can boost comfort, muscle strength, and movement, often avoiding the need for surgery.
Diverse Causes of Scoliosis
Scoliosis takes several forms:
- Structural scoliosis, the most prevalent type, often has genetic roots and emerges during early adolescence. Without treatment, it can worsen.
- Functional scoliosis can develop in adulthood due to injuries or repetitive actions.
- Pathology-related scoliosis arises from neuromuscular disorders or severe spinal injuries. Early detection and intervention are key to maintaining life quality.
Recognising Scoliosis Symptoms
Symptoms include uneven hips and shoulders, one shoulder blade sticking out more, and leaning or bending to one side. Pain around these imbalanced areas is common. While poor posture isn’t a direct cause, weak spinal muscles can exacerbate the condition. Spotting these signs early is crucial for effective treatment.
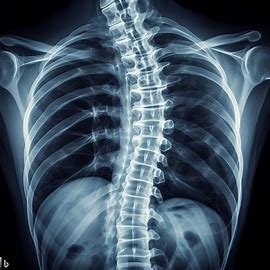
How Is Scoliosis Diagnosed?
Physiotherapists or doctors usually detect scoliosis during routine check-ups. They examine the spine, shoulders, rib cage, pelvis, legs, and feet for irregularities. X-rays, measuring the curve’s angle, help determine the condition’s severity. Significant curves, especially in adolescents, require an orthopaedic spine specialist’s evaluation. Prompt medical advice is essential for early diagnosis and treatment.
Treating Scoliosis
Scoliosis treatment varies based on its severity. Main goals include pain management, posture improvement, and halting further curvature. Non-surgical options like physiotherapy, bracing, and exercises are common. Severe cases might need surgery to straighten the spine. Consulting a healthcare professional ensures tailored treatment plans.
Orthopaedic Bracing for Scoliosis
Orthopaedic bracing plays a crucial role in treating scoliosis, particularly in adolescents whose bones are still growing. Braces aim to prevent further curvature of the spine as the patient grows. While they can’t correct existing curvature, they’re effective in halting progression. The type of brace and the duration of wear depend on the curvature’s severity and location. Regular monitoring and adjustments by healthcare professionals ensure the brace remains effective throughout the treatment period. It’s important to note that bracing is most effective when patients adhere strictly to their prescribed wear schedule.
Spinal Surgery Rehabilitation
Post-surgical rehabilitation is a critical component of recovery for patients who undergo spinal surgery for scoliosis. This phase focuses on restoring strength, flexibility, and function to the spine and surrounding muscles. A tailored rehabilitation program, often led by a physiotherapist, includes specific exercises, mobility training, and pain management strategies. The duration and intensity of rehab vary based on the individual’s condition and the type of surgery performed. Effective rehabilitation not only aids in a quicker recovery but also plays a vital role in achieving the best possible long-term outcomes for spinal health and function.
Scoliosis Prognosis
Treatment outcomes depend on the curvature’s severity, age at treatment initiation, and the chosen approach. Those with mild to moderate scoliosis can see reduced pain and spinal curvature, and improved posture. Severe cases might require braces or surgery, with specialists overseeing the process. Regular X-rays monitor progress. Treatment can greatly improve functionality and life quality.
Conclusion and What to Do
If you suspect scoliosis in yourself or your child, seek professional advice from a physiotherapist. Early detection and tailored treatment are key to managing this condition effectively.
Related Articles
- Spine Physiotherapy: How physiotherapy aids spine health.
- Posture Correction: Techniques for improving posture, essential in scoliosis management.
- Back Pain: Managing back pain, often linked with scoliosis.
- Exercise Therapy for Spinal Conditions: Exercise’s role in spinal condition treatment.
- Adolescent Spinal Conditions: Focuses on spinal issues common in adolescents, including scoliosis.
Effective Management of Upper Back Pain and Injury
Physiotherapy Insights
Introduction
Upper back pain and injury, predominantly affecting the thoracic spine, are prevalent issues causing significant discomfort and impacting daily activities. This article, infused with physiotherapy insights, aims to enlighten the general public about the causes, symptoms, and treatment options for upper back pain.


Managing Upper Back Pain
Upper back pain stems from various sources, including thoracic spine conditions, joint injuries, muscle strains, nerve irritations, and systemic diseases. Recognising these causes is vital for appropriate treatment.
Common Causes of Upper Back Pain
- Joint Injuries: Facet joint pain is a frequent issue.
- Muscle-Related Injuries: This includes back muscle pain, side strains, whiplash, muscle cramps, and DOMS (Delayed Onset Muscle Soreness).
- Bone-Related Injuries: Conditions like Scheuermann's Disease, Scoliosis, and others.
- Disc-Related Injuries: Including bulging, slipped, or herniated discs.
- Nerve-Related Pain: Such as thoracic outlet syndrome and pinched nerves.
- Systemic Diseases: These include Ankylosing Spondylitis, Fibromyalgia, and arthritis types.
Posture and Upper Back Pain
Poor posture is a significant contributor to upper back pain. Understanding and correcting sitting, standing, and sleeping postures can prevent and alleviate pain.
Physiotherapy Perspective
A physiotherapist's approach to treating upper back pain involves assessing the individual's condition and tailoring a treatment plan. This may include exercises, manual therapy, and advice on posture correction.
Latest Research and Techniques
Recent advancements in physiotherapy have introduced innovative methods for treating upper back pain. These include targeted exercises, advanced manual techniques, and utilisation of posture-improving products.
What to Do?
If you experience upper back pain, it's crucial to consult a physiotherapist for a professional assessment and personalised treatment plan.
Conclusion
Upper back pain, though common, can be effectively managed with the right approach. Understanding its causes and seeking professional physiotherapy advice are key steps towards recovery.
For more information, explore articles at PhysioWorks.
Related Articles
Joint Injuries
Muscle-Related Injuries
Bone-Related Injuries
Disc-Related Injuries
Nerve-Related / Referred Pain
Systemic Diseases
Posture Information
- Posture Syndromes
- Posture Improvement: A Guide to Improve Your Posture
- Improving Your Posture: A Guide for Better Health
- How to Achieve Perfect Posture



