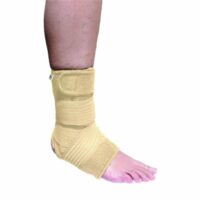
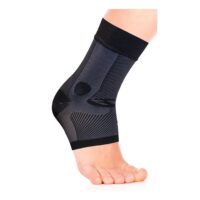
Common Heel Pain Causes
What’s Causing Your Heel Pain?
This article digs into various heel pain and injury conditions that often trouble individuals. From the well-known discomfort of plantar fasciitis to the presence of heel spurs, we’ll navigate through prevalent issues that impact our mobility.
Alongside discussions about frequently asked questions and recommended products, our exploration extends to traumatic ankle ligament injuries, tendon problems, foot injuries, bone fractures, degenerative conditions, biomechanical issues, nerve-related sources, muscle injuries, and systemic conditions. This comprehensive guide aims to provide clarity and understanding for those dealing with ankle and foot discomfort.

Heel Pain
FAQs & Products
Traumatic Ankle Ligament Injuries
Tendon Injuries
- Achilles Tendon Rupture
- Achilles Tendinopathy
- FHL Tendinopathy
- Peroneal Tendinopathy
- Tibialis Posterior Tendinopathy
Foot Injuries
Bone Injuries
- Ankle Fracture (Broken Ankle)
- Stress Fracture
- Stress Fracture Feet
- Severs Disease
- Heel Spur
- Shin Splints