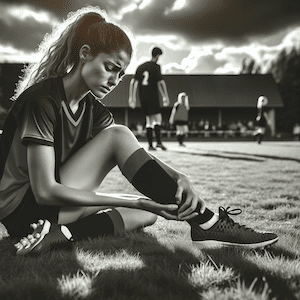Achilles Rupture
Article by John Miller
Achilles Rupture
Achilles Tendon Rupture: Understanding and Recovery
Achilles tendon ruptures are a significant concern, especially among middle-aged athletes engaging in sports like basketball, tennis, or soccer. Understanding the causes, symptoms, and treatment options is crucial for effective management and recovery. This article, from a physiotherapist’s perspective, aims to provide comprehensive insights into Achilles tendon ruptures, covering recent research and practical advice for those affected.
What Causes an Achilles Tendon Rupture?
An Achilles rupture typically occurs when the tendon snaps or pops, often without warning. This injury frequently affects middle-aged male athletes, especially during sports requiring sudden movements like jumping or pivoting. Key situations leading to a rupture include forceful push-offs, tripping or stumbling, and falls from height. A significant risk factor is tendon cell death, often a result of poorly managed tendinopathy.
Achilles Tendinopathy and Its Role
Previous Achilles tendinopathy can lead to a weakened, thin tendon, prone to ruptures. Age, lack of use, certain illnesses like arthritis and diabetes, and medications such as corticosteroids and some antibiotics increase the risk of a rupture.
Diagnosing an Achilles Tendon Rupture
Achilles tendon ruptures often go misdiagnosed, with a staggering 20%-30% rate. A thorough assessment by a healthcare practitioner, including the Thompson test, is crucial for accurate diagnosis. This test, showing high sensitivity, along with imaging techniques like ultrasound or MRI, helps confirm a rupture.
Recent Research and Treatment Advances
Recent studies suggest a conservative approach to treatment, often involving a Controlled Motion Ankle (CAM) Boot, is as effective as surgery. Surgery, though more invasive, might be necessary for re-ruptures or delayed treatment cases. The decision should be a collaborative one between patient and healthcare provider.
Non-Operative Rehabilitation
Non-operative rehabilitation for an Achilles tendon rupture focuses on gradually restoring the tendon’s strength and functionality without surgical intervention. This approach typically begins with immobilisation of the affected limb in a Controlled Motion Ankle (CAM) boot, which helps in aligning and protecting the tendon during the initial healing phase.
The rehabilitation process is carefully phased, starting with gentle range-of-motion exercises to promote flexibility, followed by strength-building exercises as the tendon heals. Physiotherapists play a crucial role in this phase, guiding patients through specific exercises tailored to their recovery stage. The ultimate goal of non-operative rehabilitation is to slowly rebuild the strength and resilience of the Achilles tendon, enabling patients to return to their normal activities and sports without risking re-injury.
This approach is often preferred for specific patient demographics or when the rupture’s characteristics make it suitable for conservative treatment.
Physiotherapy After Achilles Surgical Repair
Physiotherapy, typically starting about a week post-surgery, plays a vital role in recovery. It’s vital to avoid over-stressing the repaired tendon. A physiotherapist experienced in Achilles tendon rehabilitation can guide through this process, ensuring optimal recovery.
Recovery and Prognosis
The recovery process involves wearing a CAM brace for 6 to 12 weeks. A full return to sports might take at least 12 weeks, depending on the individual’s progress and surgeon’s advice. Some cases may take up to a year for a complete recovery, especially if complications arise.
What to Do: Seeking Professional Advice
If you suspect an Achilles tendon rupture, consult a physiotherapist or your doctor immediately. Delay can lead to a poorer prognosis. Even in cases where surgery isn’t required, a structured rehabilitation program is essential to strengthen the injured tendon and prevent further injury.
Conclusion
Achilles tendon ruptures, while serious, can be effectively managed and treated with the right approach. Understanding the causes, seeking timely diagnosis, and following a structured treatment and rehabilitation plan are key to a successful recovery. Always consult with healthcare professionals for personalised advice and treatment options.
Remember, early intervention and professional guidance are your best tools for a swift and successful recovery from an Achilles tendon rupture.
Related Articles
- Achilles Enthesopathy: Causes, Symptoms, And Treatment This article provides insights into Achilles enthesopathy, explaining its causes, symptoms, and available treatments.
- How Do You Treat Achilles Tendinopathy? Offers an overview of Achilles tendinopathy treatments, addressing common questions and concerns.
- Heel Pain Readers can explore various causes of heel pain and their links to Achilles issues.
- Running Injuries An article that discusses various running injuries, including those related to the Achilles tendon.
- Tendinopathy: Causes, Symptoms, And Effective Treatments Provides a broader understanding of tendinopathies, including those affecting the Achilles tendon.
Common Heel Pain Causes
What's Causing Your Heel Pain?
This article digs into various heel pain and injury conditions that often trouble individuals. From the well-known discomfort of plantar fasciitis to the presence of heel spurs, we'll navigate through prevalent issues that impact our mobility.
Alongside discussions about frequently asked questions and recommended products, our exploration extends to traumatic ankle ligament injuries, tendon problems, foot injuries, bone fractures, degenerative conditions, biomechanical issues, nerve-related sources, muscle injuries, and systemic conditions. This comprehensive guide aims to provide clarity and understanding for those dealing with ankle and foot discomfort.


Heel Pain
FAQs & Products
Traumatic Ankle Ligament Injuries
Tendon Injuries
- Achilles Tendon Rupture
- Achilles Tendinopathy
- FHL Tendinopathy
- Peroneal Tendinopathy
- Tibialis Posterior Tendinopathy
Foot Injuries
Bone Injuries
- Ankle Fracture (Broken Ankle)
- Stress Fracture
- Stress Fracture Feet
- Severs Disease
- Heel Spur
- Shin Splints