Anterior Ankle Impingement: Understanding and Managing the Pain
What is Anterior Ankle Impingement?
Anterior Ankle Impingement, commonly known as Footballer’s Ankle, is a condition where the front part of the ankle experiences painful compression during activities requiring ankle dorsiflexion. This condition, impacting a diverse group of individuals, warrants attention due to its prevalence and impact on mobility.
The Inner Workings of Ankle Impingement
In Ankle Impingement, the ankle joint endures damaging compressive forces during weight-bearing activities. This process leads to inflammation, joint capsule pinching, and pain. Notably, bone spurs or osteophytes may form, offering protection against repetitive stress. Understanding the biomechanical aspects is crucial for effective management.
Long-Term Impact of Untreated Ankle Injuries
An often overlooked aspect in the journey towards understanding Anterior Ankle Impingement is the role of previously untreated ankle injuries. Injuries such as ankle sprains or fractures, if not adequately treated, can lead to long-term complications, including the limitation of motion at the talocrural joint. This joint, a critical component for ankle movement, can become stiff and dysfunctional as a result of inadequate treatment of past injuries.
Stiffness and Its Consequences
Ankle stiffness, especially following sprains or fractures, is a common but significant issue. The lack of proper rehabilitation can lead to reduced flexibility and mobility in the talocrural joint, which plays a pivotal role in smooth and pain-free ankle movements. Over time, this stiffness can alter the mechanics of the ankle, placing abnormal stress on different parts of the joint.
Predisposition to Anterior Ankle Impingement
When the talocrural joint is compromised, individuals are at a higher risk of developing conditions like Anterior Ankle Impingement. The altered ankle mechanics due to previous injuries can lead to increased compression at the front of the ankle, especially during activities requiring dorsiflexion. This compression is a primary factor in the onset of impingement symptoms.
The Importance of Comprehensive Treatment
This information underscores the importance of seeking comprehensive treatment for any ankle injury, no matter how minor it may seem. Early and effective intervention, including physiotherapy and appropriate exercises, not only aids in the proper healing of the initial injury but also plays a crucial role in preventing long-term complications like Anterior Ankle Impingement.
Individuals who have suffered past ankle injuries should be vigilant about any changes or discomfort in their ankles, particularly during activities that strain the joint. Consulting with a physiotherapist for a proper assessment and treatment plan is vital in these scenarios.
By understanding the link between untreated ankle injuries and the development of Anterior Ankle Impingement, we can better appreciate the need for thorough treatment and rehabilitation of ankle injuries. This approach not only addresses the immediate injury but also safeguards against future joint complications, ensuring long-term ankle health and functionality.
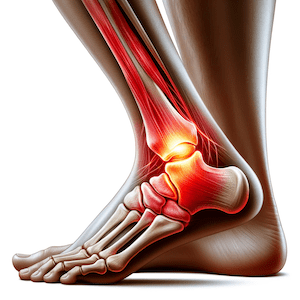
What Does an Ankle Impingement Feel Like?
The symptoms of Anterior Ankle Impingement typically include pain at the front or side of the ankle. This pain often follows a previously healed sprained ankle but the impingement pain persists. Additionally, weakness or giving way or instability in the ankle is common.
A clear indication of impingement is pain when the ankle is moved into dorsiflexion in weight-bearing (knee bending forwards over your foot). The symptoms of Anterior Ankle Impingement usually develop gradually rather than suddenly, and there is often a clicking sound at the front of the ankle during walking or rotating the foot.
Does Anterior Ankle Impingement Hurt to Walk?
It can be painful to walk on uneven surfaces or uphill, as these actions can compress the front of the ankle, leading to a pinching sensation. Running, jumping, and activities like kicking a ball can exacerbate the pain. It’s also noted that symptoms are typically eased by plantarflexing the foot. Walking down stairs is often limited by the ankle range so the person often twists the foot outwards to compensate for the lack of range.
Moreover, Anterior Ankle Impingement is commonly associated with a decrease in overall ankle range of motion, particularly affecting dorsiflexion. This limitation can be accompanied by pain and inflammation.
What is the Test for Anterior Ankle Impingement?
A physiotherapist or sports doctor assesses Anterior Ankle Impingement through a detailed medical history and physical examination. Imaging tests, when necessary, provide a clearer picture of the internal ankle structure, aiding accurate diagnosis.
How Do You Fix Anterior Ankle Impingement?
Physiotherapy plays a pivotal role in the treatment of Anterior Ankle Impingement. It offers a non-invasive, effective approach to manage and alleviate symptoms. Manual techniques used by physiotherapists, such as joint mobilisation and soft tissue massage, are particularly beneficial. These techniques not only help in reducing pain and swelling but also improve joint mobility.
Joint mobilisation involves gentle movements of the ankle joint by the physiotherapist to restore normal joint mechanics and function. This technique is effective in breaking down the stiffness that often accompanies impingement. Soft tissue massage, on the other hand, focuses on the muscles and ligaments around the ankle. It helps in reducing muscle tightness and improving blood flow to the affected area, which accelerates the healing process.
Exercise in Restoring Normal Ankle Motion
Exercises form the cornerstone of recovering from Anterior Ankle Impingement. As pain and swelling decrease, physiotherapists introduce specific exercises aimed at restoring the normal range of motion in the ankle. These exercises are designed to gradually stretch and strengthen the ankle joint, improving its functionality.
Stretching exercises focus on the calf muscles, which play a crucial role in ankle movement. By improving the flexibility of these muscles, the ankle can move more freely, reducing the risk of further impingement. Strengthening exercises, meanwhile, target the muscles around the ankle to provide better support and stability to the joint.
Balance and proprioception exercises are also integral to the recovery process, especially for athletes. These exercises help in retraining the ankle to respond to changes in terrain and movement, which is crucial in preventing recurrent ankle issues.
By combining these exercise regimes with manual techniques, physiotherapy offers a holistic approach to treating Anterior Ankle Impingement. It not only addresses the immediate symptoms but also works towards long-term prevention of recurrence. This comprehensive approach ensures that individuals can regain their full range of ankle motion and return to their normal lifestyle or sporting activities with confidence.

Proactive Steps and Seeking Help
It’s imperative to consult a physiotherapist, orthopaedic surgeon or sports doctor for a tailored treatment plan. They offer professional guidance on managing the condition and advice on preventative measures to avoid recurrence.
Conclusion
Anterior Ankle Impingement, while a common issue, can be effectively managed and treated with the right approach and professional guidance. Early detection, consistent treatment, and following professional healthcare advice are key to overcoming this condition.
Feel free to consult your physiotherapist or ankle specialist for any concerns or questions about Ankle Impingement.
Related Articles
- Common Causes of Ankle Pain – This article discusses various conditions and injuries leading to ankle discomfort, such as sprains and degenerative diseases, which are relevant to understanding Anterior Ankle Impingement.
- Sprained Ankles – It covers common issues like sprained ankles, which are crucial to understand for anyone exploring ankle impingements and their causes.
- Posterior Ankle Impingement – This article discusses a condition causing pain at the back of the ankle, especially relevant for understanding different types of ankle impingements.
- High Ankle Sprain and Syndesmosis Injuries – High ankle sprains are significant to note as they can impact the same region as anterior ankle impingement, offering a broader perspective on ankle injuries.
- Common Football Injuries – This article provides a comprehensive guide to various injuries associated with football, including minor sprains to severe conditions. It also discusses the role of sports physiotherapy in injury management and prevention, which is crucial for understanding and dealing with “Footballer’s Ankle”
- Anterior Shin Splints: Key Symptoms, Managing, Tips & Care – Readers can learn about shin splints, a condition related to the mechanics of the foot and ankle, which might be relevant for those experiencing Anterior Ankle Impingement.
- Ankle Arthritis – It discusses how arthritis in the ankle affects joint pain and stiffness, which could be relevant for readers exploring Anterior Ankle Impingement.
Common Causes of Ankle Pain
Introduction
Welcome to our detailed guide on the common causes of ankle pain. As physiotherapists, we understand how various conditions and injuries can lead to discomfort in your ankle. From sprains to degenerative diseases, this guide aims to provide clear insights for the general public on navigating these issues.


Sprained Ankles and Syndesmosis Injuries
Sprained ankles, including syndesmosis injuries, are among the most common issues we encounter. These injuries can range from mild ligament stretches to severe tears, impacting your mobility and quality of life. Understanding the specifics of each type is crucial for effective treatment and timely recovery.
Ankle Tendinopathies
Tendinopathies, such as those affecting the Achilles and tibialis posterior tendons, are common in active individuals. These conditions arise due to overuse or trauma, leading to pain and swelling in the affected area. Targeted physiotherapy can significantly aid in recovery and prevent future injuries.
Posterior Ankle Conditions
Conditions like posterior ankle impingement and retrocalcaneal bursitis can cause significant pain, especially during physical activities. Recognising these conditions early and starting appropriate treatment is vital for maintaining ankle health and functionality.
Ankle Arthritis
Arthritis in the ankle, often a result of wear and tear or injury, leads to joint pain and stiffness. Early intervention and proper management, including physiotherapy, are essential to slow its progression and manage symptoms effectively.
Biomechanical Conditions
Abnormal foot and ankle biomechanics can lead to various issues, from pain during weight-bearing to nerve compression. Understanding and treating these conditions are crucial for restoring normal function and preventing further complications.
Systemic Conditions That May Cause Ankle Pain
Systemic diseases such as rheumatoid arthritis can manifest as ankle pain. It's important to address these underlying conditions to effectively manage ankle symptoms.
Conclusion
Ankle pain can arise from a multitude of causes, each requiring a unique approach to treatment. If you're experiencing ankle discomfort, we recommend consulting a physiotherapist or doctor for a thorough evaluation. A personalised care plan can significantly improve your quality of life and mobility.
Related Articles
- Sprained Ankle Treatment & Recovery Guide - This article provides comprehensive information on managing pain and inflammation for a sprained ankle, including initial RICE steps and exercises for restoring mobility.
- Anterior Ankle Impingement: Causes, Treatments, Tips & Guide - Offers insights into the causes of anterior ankle impingement, its treatments, and practical tips for management.
- Posterior Ankle Impingement: Causes & Treatments - Explains the condition of posterior ankle impingement, its causes, and available treatment options.
- Tibialis Posterior Tendinopathy - Discusses the condition affecting the tibialis posterior tendon, symptoms, and implications for foot arch pain and ankle stability.
- Achilles Tendinopathy - Answers frequently asked questions about foot and ankle pain associated with Achilles tendinopathy and provides an overview of tendon injuries.
- How To Strap An Ankle - Guides on the correct techniques and types of tape for ankle strapping to prevent or manage ankle injuries.
Foot, Ankle & Heel Pain FAQs
Introduction
Welcome to PhysioWorks' comprehensive FAQ page on Foot, Ankle, and Heel Pain. Our expert physiotherapists are here to guide you in managing and overcoming discomfort. We’ve organised the FAQs into categories, each with a brief overview and links to in-depth articles, making navigation and understanding easier for you.


Foot Pain
Step into the various causes of foot pain and learn effective ways to relieve discomfort. Understand the impact of activities like barefoot running.
Ankle Injuries
Explore common ankle injuries and how to address them. From sprains to ligament damage, find out the best practices for care and prevention.
Heel Pain
Uncover the reasons behind heel pain and the effective treatments available. This section is particularly useful for understanding conditions like plantar fasciitis and heel spurs.
Achilles Pain
Find out how to manage and treat Achilles tendinopathy, a common concern for athletes and active individuals.
Shin Pain
Learn about shin splints, their causes, and how to alleviate this common issue, especially among runners.
Youth Injuries
Gain insights into youth leg injuries, including growing pains and heel issues in children.
Balance & Proprioception
Enhance your balance and proprioception with our professional advice and exercises.
Related Articles
- Sprained Ankle Treatment & Recovery Guide: Offers detailed advice on how to manage sprained ankles, including immediate recovery steps and physiotherapy treatments.
- Ankle Pain: Effective Management And Treatment Options: Discusses various conditions leading to ankle pain and outlines effective treatment strategies, highlighting the role of physiotherapy in pain reduction and mobility improvement.
- Plantar Fasciitis: Provides an overview of plantar fasciitis, including common causes, treatment options, and related conditions like peroneal tendinopathy and Achilles tendinopathy.
- Achilles Tendinopathy: Focuses on the causes of Achilles tendinopathy, its impact on heel pain, and a range of treatment and prevention strategies.
- Ankle Strapping: Complete Guide To Injury Prevention: Explains the benefits of ankle strapping as a preventative measure against injuries, with a focus on techniques and materials.
- Heel Pain: Explores various causes of heel pain, including tendon injuries, foot injuries, bone injuries, and systemic conditions, alongside recommended treatments.